Home / Journal / Oral Health and Dental Studies
Clinical Application of Violet LED In-office Bleaching with or without Traditional Systems: Case Series
dental bleaching dentin sensitivity hydrogen peroxide carbamide peroxide
Matheus Kury, Bruna de Almeida Resende, Daylana Pacheco da Silva, Erica Eiko Wada, Fernanda de Moura Antonialli, Marcelo Giannini, and Vanessa Cavalli
DOI: 10.31532/OralHealthDentStud.2.1.001 28 Jan 2019
Abstract
Objective: This study evaluated the efficacy and tooth sensitivity of bleaching with the novel violet LED light used in different in-office approaches.
Clinical Considerations: Three patients were submitted to anamnesis, clinical and radiographic exams and to different bleaching protocols and materials.
Case report I: Violet LED light was applied in 20 irradiations of 1 minute at 30-s intervals without the use of peroxide agents. After eight appointments with 4 or 7-day intervals, no tooth sensitivity (TS) was reported and color changed from A2 to A1 and from B3 to A2 in upper central incisor (tooth 11) and upper canine (tooth 13), respectively.
Case report II: The same protocol established for violet LED light application was used and associated with 37% carbamide peroxide in three appointments at intervals of 7 days. Color changed from A3,5 to B2 (tooth 13), and provoked TS was reported.
Case report III: 35% hydrogen peroxide was associated with the same violet LED regimen and number of sessions. Although spontaneous TS was reported in low levels, color changed from A2 to B1 (tooth 11) and from A3 to B1 (tooth 13).
Conclusion: Although the three treatments promoted different bleaching responses, in vitro and in vivo investigations of the violet LED protocols are still necessary. In addition, the fact that the sensitivity levels obtained are compatible with conventional bleaching treatments demonstrated that violet LED light is possibly adequate for clinical use.
Clinical Significance: Bleaching of vital teeth with violet LED with or without peroxide agents exhibited acceptable clinical results and low sensitivity responses.
Keywords
Dental bleaching, dentin sensitivity, hydrogen peroxide, carbamide peroxide.
Introduction
In-office tooth bleaching is commonly accomplished with the application of high-concentrated oxidative agents on the enamel surface.1 As a consequence, patients may report tooth sensitivity during or for a few days following the procedure.2 In comparison to at-home therapy, this clinical symptom is a drawback of in-office technique, since some patients may quit the treatment after experiencing intense sensitivity.3
Alternative bleaching therapies have been described as an attempt to fasten in-office bleaching results.4,5 The in-office association of LED/laser (blue wavelength) with high-concentrated hydrogen peroxide agents, for instance, was used as an alternative to accelerate the peroxide reaction.6 Although controversial, some authors reported that light may have catalyzed the peroxide reaction, reducing the required session time to reach a desirable bleaching outcome.7,8 Moreover, photocatalysts such as TiO_N have been added into low-concentrated bleaching gels in order to enhance the free radicals release and, in turn, result in comparable color change to 35-38% HP gels with lower sensitivity levels.9
Recently, a novel light source with a violet LED has been introduced, aiming to promote bleaching without the use of chemical agents. According to the manufacturer, this device irradiates visible violet light in the wavelength of 405 nm, and this spectrum could be capable of bleaching teeth in the absence of any peroxide agent.10 In order to accelerate bleaching, the manufacturer also suggests the association of the violet LED light with either high-concentrated carbamide or hydrogen peroxide aiming to reduce the length of clinical appointments.10 Therefore, violet LED could be applied alone or associated with carbamide and hydrogen peroxide.
Clinical reports demonstrated the violet LED light efficacy alone or associated with carbamide peroxide.11–14 Thus, the irradiation of violet LED light with no peroxide association or less concentrated agents than hydrogen peroxide may be an interesting option for patients with severe tooth sensitivity. Moreover, the combination of violet LED with the chemical agents may reduce chair-side appointments, costs and patient’s discomfort.15
In view of these facts, this report shows in a series of cases the contrast of the effectiveness of the three whitening systems.
Case Series
After ethical approval by the Piracicaba Dental School Ethical and Research Committee, patients designated to bleaching signed an informed consent. Eligibility criteria evaluation for violet LED bleaching protocols underwent with a detailed anamnesis, in which patients were questioned about their previous medical and dental history. Patients had to answer an inquiry on dietary and oral health habits. Moreover, volunteers were submitted to clinical and radiographic exams and periodontal evaluation. The inclusion criteria comprised periodontal health, absence of caries lesions, enamel cracks or exposed dentin. Baseline color evaluation of upper canine required a minimum shade of A3, and patients must not had been undergone tooth bleaching in the previous three years. If one of the assumptions were disrupted or if the patient underwent previous bleaching treatment, then the exclusion criteria were applied.
The three patients selected were submitted to different bleaching protocols:
- Case Report I – violet LED light
- Case Report II – violet LED light associated with 37% carbamide peroxide (CP)
- Case Report III – violet LED light associated with 35% hydrogen peroxide (HP).
The bleaching agents used in the three cases are described in table 1 along with the manufactures instructions. The number of bleaching appointments and application of the bleaching agents were performed according to each technique and summarized in table 2.
Table 1. Description and composition of the physical and chemical agents used in the clinical cases and their respective manufacturer’s instructions
| Product | Basic composition | Manufacturer's instruction |
| Bright Max Whitening - BMW (MMOptics, São Carlos, SP, Brazil) | Four light emitting diode lamps in violet wavelength (405 nm) positioned in a curved acrylic tip. | Applied for 30 min (20 consecutive 1-min irradiation at 30-s intervals) associated or not with high-concentrated bleaching agents. When no agent is applied, 4 to up to 10 appointments are indicated. Three sessions is the limit indicated when associated with peroxide agents. |
| Whiteness Super Endo (FGM, Joinville, SC, Brazil) | 37% carbamide peroxide, neutralized carbopol, inert filler, glycol and deionized water. | Used in walking bleaching technique within non-vital teeth bleaching. It is placed into pulp chamber and must be evaluated and replaced if necessary in every three to four days up to eight times. |
| Whiteness HP (FGM, Joinville, SC, Brazil) | 35% hydrogen peroxide, dyes, glycol, inert filler, deionized water and thickener. | Indicated for vital teeth bleaching with three 15-min applications. 7-day interval required between up to four sessions. |
Table 2. Bleaching protocols set for each of three vital bleaching case reports
| Case Report | Bleaching Protocol |
| I | 20 consecutive 1-min violet LED irradiation with 30-s intervals were performed in eight appointments with 4 to 7-day intervals. The light tip distance from the upper and lower arches was standardized using a tripod, which set the acrylic tip 8-mm distant from the teeth. |
| II | Three appointments of a single application of 37% carbamide peroxide gel on the teeth surface was performed during 30 min concomitantly with the Violet LED irradiations. The distance of the LED tip was also defined as the first protocol. 7-day intervals were done among sessions. |
| III | Three appointments of a 35% hydrogen peroxide were also applied in the teeth surface for 30 min in a single performance. During all the application time, the violet LED was activated and positioned as the first and second protocols. 7-day intervals were done among sessions. |
Color evaluation was registered in the upper right central incisor (11) and upper right canine (13) at each appointment with color shade guide Vitapan Classical A1–D4 (Vita, Bad Sackingen, Germany) and hand spectrophotometer (VITA Easyshade, Bad Sackingen, Germany). Two evaluators were calibrated in standardized light, temperature and pressure conditions. Previous appointments were performed with a certain number of patients to determine parameters for differences among scale tabs for both calibrators, and for standardizing the use of the spectrophotometer. In addition, tooth sensitivity (TS) was assessed by means of a Visual Analogue Scale (VAS), in which, patient is able to classify pain according to the numerical range: 1 (lowest TS) to 10 (highest TS). The VAS measured tooth sensitivity immediately and 24 h after the bleaching session. The color change and TS results for each volunteer are described in table 3.
Table 3. Upper right incisor (11) and canine (13) shades measured with spectrophotometer/visual shade guide before and after bleaching, and intensity tooth sensitivity values obtained by volunteers’ reports by means of a visual analogue scale during sessions and their intervals.
| Volunteer | Initial Shade | Final Shade | TS intensity(sessions) | TS intensity(sessions) |
| LED | (11) A2; (13) B3 | (11) A1; (13) A2 | 0 | 0 |
| LED/CP | (11) A1; (13) A3.5 | (11) A1; (13) B2 | 0 | 1st = 0 - 2nd = 4 - 3rd= 3 |
| LED/HP | (11) A1; (13) A3 | (11) B1; (13) A1 | 0 | 1st = 1 - 2nd = 2 - 3rd= 3 |
Case Report I
A 19-year old male patient underwent the preliminary exams, had no previous history of tooth sensitivity and was considered eligible to be submitted to bleaching. The initial color of the teeth was registered with the color shade guide and spectrophotometer. The upper right central incisor (11) and canine (13) were A2 and B3, respectively (Figures. 1A and 1B) and the treatment proposed was in-office whitening using the violet LED light source without the use of chemical whitening agent.
Initially, dental prophylaxis was carried out in all appointments and a gingival barrier with a light-cure resin paste (Top Dam, FGM, Joinvile, SC, Brazil) was applied on the free gingival margin of teeth exposed to bleaching (14–24), in order to avoid thermal damage or dryness of the gingival tissue. The patient’s eyes were protected with blue-blocker glasses during the entire procedure. This gingival barrier was performed from maxillary and mandibular molar to molar of the opposite side with a 2-mm thickness. The flowable resin was light-cured for 20 s (Valo, Ultradent, South Jordan, UT, USA). Following the instructions (MMOptics Electronic Equipment, São Carlos, SP, Brazil), violet LED light irradiated the upper front arch for 1 minute followed by a 30-s interval. This procedure was repeated 20 times and the total light delivery was 20 min, and the clinical session endured 30 min. The power of the LED, which was used in the three report cases, is 1,200 mW. The calculated emittance of the light source is approximately 112 mW/cm2. Thus, the radiant energy of the violet LED is 6.7 J per cycle (60 s). Within the intervals, moisture gauze was applied over teeth and gingival margins in order to rehydrate the exposed enamel and soft tissues.
Figure 1. Aspect of the dental elements before being submitted to bleaching with violet LED only.
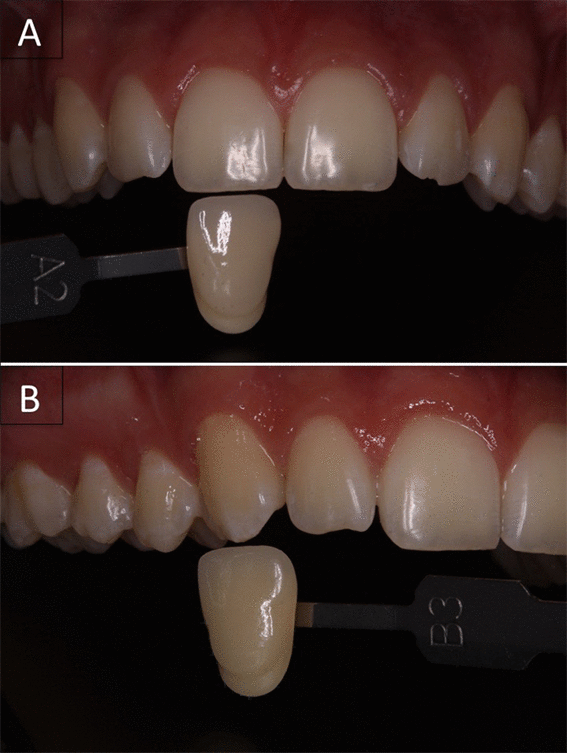
Before the LED irradiation, upper right central incisor was detected with shade A2 and the upper right canine with shade B3.
Eight sessions were performed at intervals of 4 to 7 days and at the end of bleaching, color shade was re-evaluated. The color of upper right central incisor (11) and canine (13) was reduced from A2 to A1 and from B3 to A2, respectively (Figures. 2A and 2B). During and after treatment, according to the VAS scale, patient reported no levels of tooth sensitivity.
Figure 2. Final color measurement of dental elements after bleaching with violet LED only.
After the protocol using LED not associated with any chemical agents, the upper right incisor shade ranged from A2 to B1 and the upper right canine from B3 to A2.
Case report II
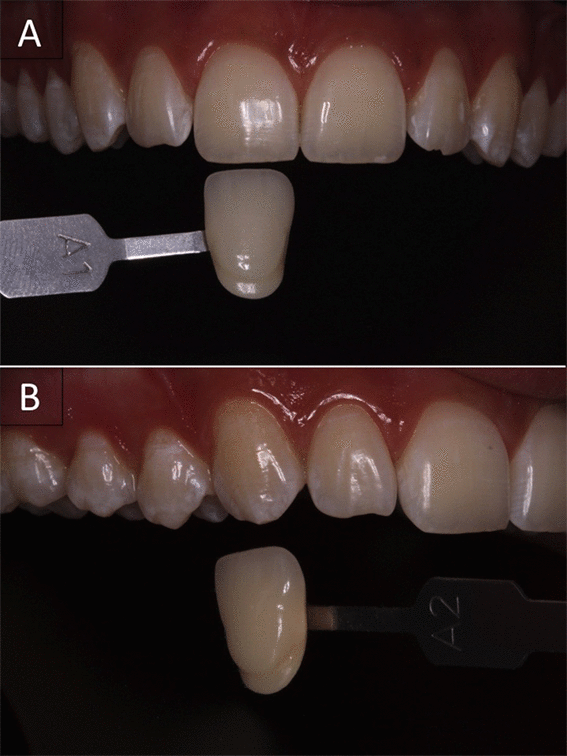
A 24-year-old male patient fulfilled the preliminary conditions of eligibility. This patient was submitted to bleaching with violet LED light associated with 37% carbamide peroxide (Whiteness Super-endo, FGM, Joinville, SC, Brazil). The upper right central incisor and upper right canine exhibited color shade A1 and A3.5 (Figures. 3A and 3B), respectively, according to the color scale and manual spectrophotometer.
Figure 3. Dental elements before bleaching with high-concentrated carbide peroxide associated with violet LED light.
At the first appointment, the color evaluation indicated that upper right incisor and canines of the patient were A1 and A3,5 respectively.
Prophylaxis was performed and the gingival tissues were protected with a light-curing gingival barrier as described in case I (Top Dam, FGM, Joinville, SC, Brazil). The bleaching agent was applied in 3 sessions of 30 min each (Figure. 4), directly from the syringe in which the transparent gel is marketed. The gel was applied in both maxillary and mandibular teeth, among second premolars, covering the entire enamel buccal surface with a thickness of approximately 1 mm. The LED was applied simultaneously to CP application, following the protocol established for violet LED light application (20 light irradiations for 1 min followed by a 30-s interval). Three bleaching sessions were undertaken at a 7-day interval. At the end of bleaching treatment, the upper right central incisor (11) kept the shade A1 and the upper right canine (13) exhibited color change from A3.5 to B2 (Figures. 5A and 5B). The VAS exhibited level 4 and 3 of induced sensitivity from 1 up to 24 h after the second and third appointment, respectively.
Figure 4. The ideal condition of the violet LED use in patients.
The violet LED light positioned at 8-mm distance from the patient's arches protected with gingival barrier. High-concentrated carbide peroxide is placed on the enamel surface during all light activation as the protocol described in the case report.
Figure 5. Aspect of dental elements after bleaching with carbide peroxide light-activated.
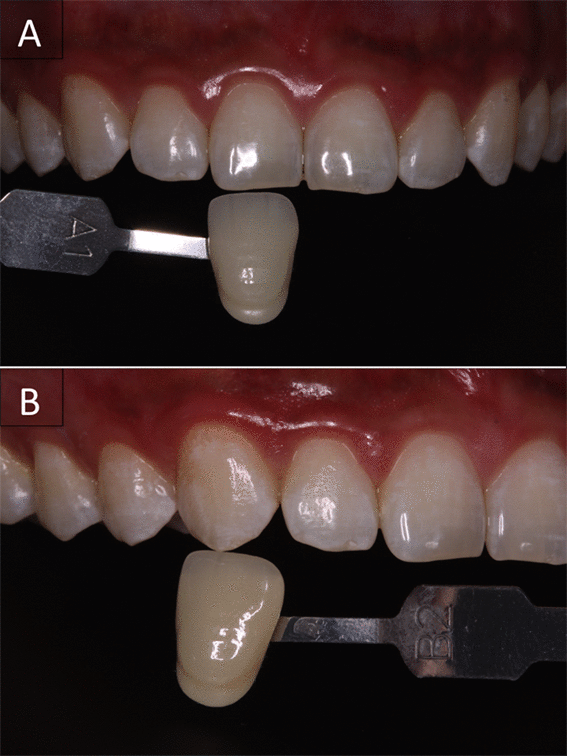
The final evaluation of the patient indicated that his upper right central incisor did not change in terms of shade. However, the upper right canine ranged from A3,5 to B2.
Case Report III
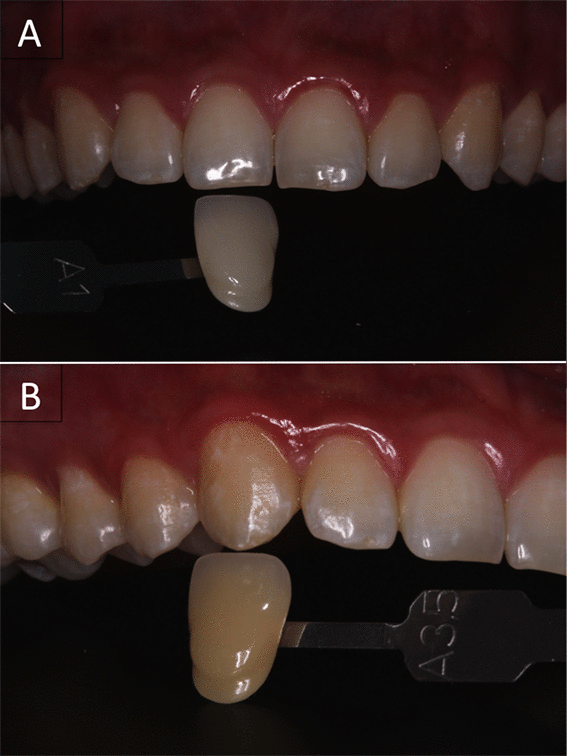
A 23-year-old male volunteer was submitted to detailed anamneses, clinical and radiographic exams as previously described. Bleaching protocol adopted for him was the association of violet LED light with 35% hydrogen peroxide (Whiteness HP, FGM, Joinville, SC, Brazil). The initial color of the central incisor and upper right canine were A2 and A3, respectively, according to the color shade evaluations (Figures. 6A and 6B).
Figure 6. Initial condition of patient's upper arch before being submitted to bleaching with LED and HP.
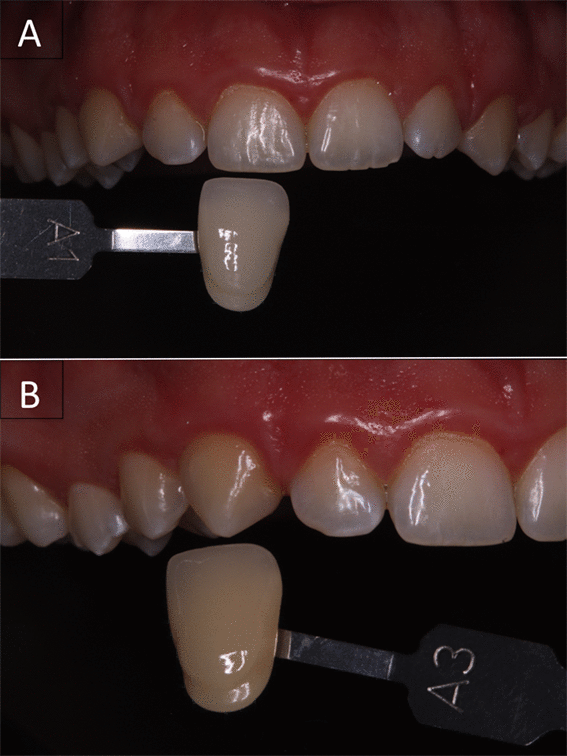
Upper right central incisor exhibited shade A1 and upper right canine A3.
Initial procedures previous to bleaching described in case I and II were also performed for this case. Hydrogen peroxide and thickener were mixed until becoming a homogenized gel with a reddish aspect. The gel was placed on enamel buccal surface on the same area described for case II, and it was maintained for 30 minutes. During the first minutes of gel application, the color changed for transparent. Violet LED was applied following the protocol settled by the manufacturer. After 3 bleaching appointments (Figure. 7), the upper right central incisor and upper right canine changed from A1 to B1 and from A3 to B1, respectively (Figures. 8A and 8B). After 24 h of the first and second appointments, patient reported levels 1 and 2 of induced tooth sensitivity, respectively, and after the third appointment, level 3 of spontaneous tooth sensitivity.
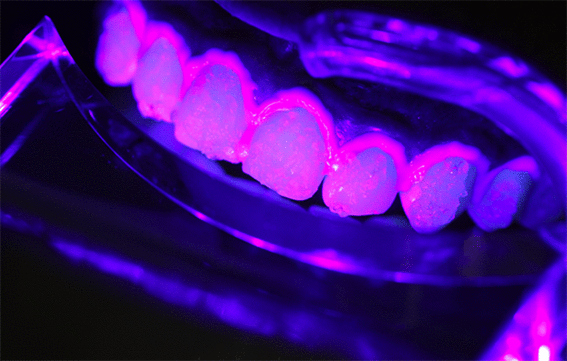
Figure 7. The view of an ideal position of the violet LED towards patient’s arches.
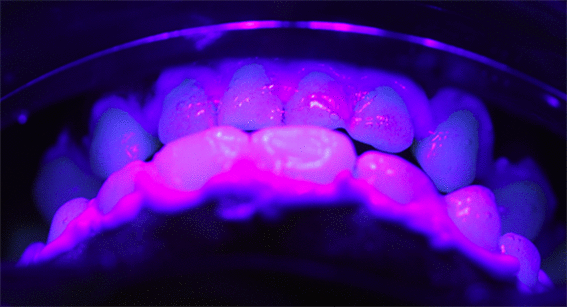
Patient's teeth protected with gingival barrier and 35% hydrogen peroxide associated with the violet LED light fixed 8-mm away from the arches.
Figure 8. Final condition of the patient's upper teeth after bleaching with high-concentrated hydrogen peroxide associated with the LED.
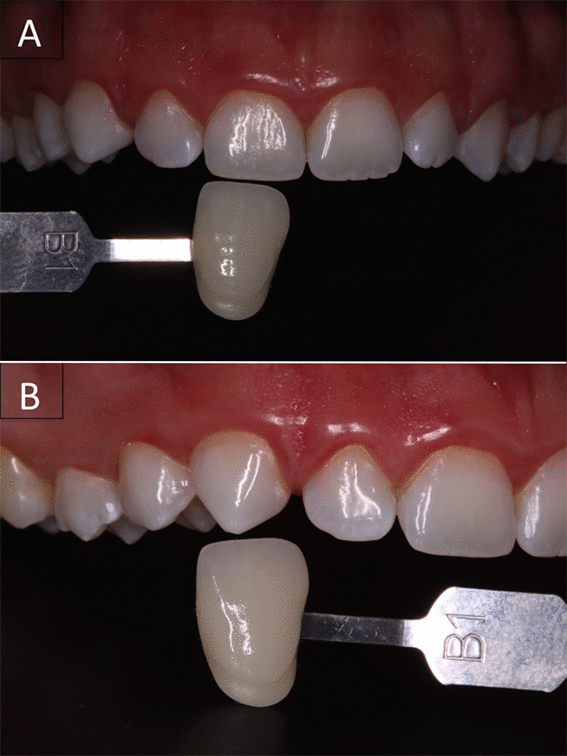
After bleaching therapy, upper right incisor and canine presented shade B1. However, the change was more noticeable for canine, whose shade began at A3.
Discussion
Although color shift was observed in different intensities among patients, all techniques using violet LED light were capable of bleaching teeth. In addition, we could notice that the TS intensities caused by bleaching with HP or CP peroxide gels were similar to previous clinical trial, in which, 35% HP associated with LED promoted intense TS in comparison to light-activated 20% HP.2 Other clinical trials pointed out that TS is a common adverse event of bleaching without light activation, and even when its intensity was either moderate or severe, patients did not suspend treatment16,17 and did not present permanent sensitivity.18
As expected, the intensity of color alteration was ranked according to the presence and the concentration of peroxide agent. However, it is noteworthy that the application of violet LED light itself was capable of promoting color alteration of upper central incisor and canine. Although it is known that dehydration may increase enamel brightness19, follow-up appointments may indicate whether factors such as rehydration and regular diet would cause a shade rebound. Besides this, Rastelli et al. 13 stated that the absorption peak of pigments is at violet wavelength, which could explain the action of the light on the extrinsic staining of teeth. The manufacturer of the violet LED light indicates 4 to 10 appointments with bleaching purpose when light is applied without the chemical agent. Since this is a far-reaching interval and there is no evidence supporting this treatment decision, the shade of teeth evaluated was checked at the beginning of each bleaching appointments in order to estimate the treatment progress. Because no color change was detected after the fifth appointment, eight appointments were established.
On the contrary, protocols associating light source with peroxide agents were expected to promote color change due to the oxidative reaction promoted by hydrogen peroxide.20 It is known that hydrogen peroxide may diffuse through enamel and reach dentin, where its by-products would break the chains of the organic compounds that stain teeth, the chromophores.21 The manufacturer claims that violet LED would enhance and hasten in-office bleaching with peroxide gels. The literature indicates that light could increase the temperature of the gel, thereby enhancing the energy within the gel. As a consequence, molecular collision and more free radicals formation would be favored, increasing the interaction with chromophores.21 Further randomized clinical studies may provide the comparison among LED-activated HP and CP to correspondent groups without light activation, addressing whether the violet LED is playing a role on chemical reaction of the bleaching gels.
Besides this, it was previously reported that light irradiation enhances the energy of the staining molecules, which may increase their reactivity with the oxidative agent.22 On the other hand, evidence implies that violet LED light has lower penetration capability through teeth. 23 Even though a recent systematic review stated that blue LED, LED/laser and halogen lamp have no impact on the final result of in-office bleaching using low or high-concentrated agents,1 included articles differed among protocols and light sources types. Therefore, research on the novel violet LED with its specific irradiation cycles is paramount to determine efficacy and safety on in-office bleaching.
In spite of the bleaching gels used for these protocols, recent researches have investigated the incorporation of TiO_N nanoparticles on low-concentrated bleaching gels that should be activated by ultraviolet light.5,24 However, the harmful impact of this radiation on health raises a disadvantage of this treatment option. In order to overcome such limitation, a clinical trial evaluated the association of blue LED with 15% HP doped with TiO_N, showing statistical comparable results with 35% HP and lower tooth sensitivity for 15% HP.9 The authors explain the results due to HP catalyzation by the nanoparticle, and a shorter wavelength than blue is expected to enhance this color change. Thus, the application of violet LED with specific gels should be investigated.
The lack of information available about the topic also raises the discussion on the safety of violet LED light. As it is believed that the association of a light source with the peroxide would accelerate its decomposition, peroxide diffusion towards pulp chamber may be influenced. 25 Such event could be clinically perceptible as the intensity of tooth sensitivity would increase.3 However, the concentration of the agent should be taken into account, since the higher the peroxide concentration, the more intense the tooth sensitivity.26,27 We therefore assume, that concentration played the major role on the sensitive levels registered, not light irradiation. Indeed, the correlation among high-concentrated HP and LED/laser activation in terms of sensitivity intensity is controversial since some authors showed that this association resulted in higher TS levels,28,29 while others detected no difference between groups with or without light.2,30
The decision on not replenishing the gels concerns that this would lead to higher sensitivity. Nevertheless, Vildósola et al. 31 showed that light-activated 6% HP with titanium dioxide in a single 36-min application resulted in equal sensitivity levels than three 12-min application. Moreover, Martins et al.32 reported that refreshing 38% HP after 20 min resulted in similar TS of the same gel applied during uninterrupted 40 min. In both studies the same efficacy was found among groups, which confirms that the single gel application on cases II and III did not affect the efficacy and safety of in-office bleaching.
Moreover, it should be kept in mind that the use of a light source could increase pulp chamber temperature.33 Violet LED device establishes a protocol of 30-second intervals among the 1-min LED irradiation that aims to decrease temperature promoted by light irradiation. At this interval, teeth must be rehydrated with moisture gauze in order not to harm pulp tissue. Soares et al.34 demonstrated in vitro that violet irradiation increases pulp temperature up to 2 °C, but this raise could be reversed with rehydration, not leading to permanent damage to pulp.
Although randomized-controlled clinical trials are indicated to compare risk and the intensity of tooth sensitivity among treatments and ensure the safety of bleaching,35 the cases reported herein showed that the correct patient selection is crucial for the treatment success. The three patients submitted to bleaching exhibited excellent oral health, with healthy periodontal condition and no adverse changes of dentin-pulp complex. When planning to use light irradiation with or without peroxide agents, clinicians must evaluate anatomy of the tooth, tooth sensitivity responses and the presence of adhesive restorations36 in order not to overexpose compromised teeth to agents that could exacerbate tooth sensitivity and trigger permanent pulp damage.37,38
Overall, the three case reports promoted satisfactory results for patients submitted to bleaching. These clinical cases showed that the new technology may reduce application time and diminish concentration or eliminate the presence of peroxide. However, limitations such as the lack of comparison with only gel-containing protocols and replication of these cases in more patients cannot precisely ensure the supplementary effect of violet LED on bleaching gels. Further clinical trials might address questions concerning short and long-term color change outcomes within a considerable sample size.
Conclusion
According to the limitations of the reports, these case series showed efficient in-office protocols with different levels of bleaching. Even though LED itself promoted color change, the presence of carbamide and hydrogen peroxide provoked higher bleaching efficacy. In addition, sensitivity levels were comparable with previous studies in the literature.
Acknowledgments
This study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior - Brasil (CAPES) - Finance Code 001. The authors thank CNPq (#132132/2017-6), FAPESP and CAPES (#2017/08625 and #2017/24847-3) for student fellowships and FAPESP for a research grant (#2017/23841-1).
References
- Maran BM, Burey A, de Paris Matos T, Loguercio AD, Reis A. In-office dental bleaching with light vs. without light: A systematic review and meta-analysis. J Dent. 2018;70: 1–13.
- Mena-Serrano AP, Garcia E, Luque-Martinez I, et al. A Single-Blind Randomized Trial About the Effect of Hydrogen Peroxide Concentration on Light-Activated Bleaching. Oper Dent. 2016;41(5): 455–464.
- Markowitz K. Pretty painful: why does tooth bleaching hurt? Med Hypotheses. 2010;74(5): 835–840.
- Langsten RE, Dunn WJ, Hartup GR, Murchison DF. Higher-concentration carbamide peroxide effects on surface roughness of composites. J Esthet Restor Dent. 2002;14(2): 92–96.
- Martín J, Vildósola P, Bersezio C, et al. Effectiveness of 6% hydrogen peroxide concentration for tooth bleaching—A double-blind, randomized clinical trial. J Dent. 2015;43(8): 965–972.
- Sulieman M. An overview of the use of lasers in general dental practice: 2. Laser wavelengths, soft and hard tissue clinical applications. Dent Update. 2005;32(5): 286–288, 291–294, 296.
- Ontiveros JC, Paravina RD. Color change of vital teeth exposed to bleaching performed with and without supplementary light. J Dent. 2009; 37(11):840-847.
- Hayward R, Osman Y, Grobler SR. A clinical study of the effectiveness of a light emitting diode system on tooth bleaching. Open Dent J. 2012; 6:143-147.
- Bortolatto JF, Pretel H, Floros MC, et al. Low Concentration H(2)O(2)/TiO_N in Office Bleaching: A Randomized Clinical Trial. J Dent Res. 2014;93(7 Suppl): 66S–71S.
- MMOptics. Sugestão de protocolos de utilização - Bright Max Whitening. 7a ed. Retrived from: https://mmo.com.br/pt-br/produtos/odontologia/bright-max-whitening
- Lago ADN, Ferreira WDR, Furtado GS. Dental bleaching with the use of violet light only: Reality or Future? Photodiagnosis Photodyn Ther. 2017;17: 124–126.
- Panhoca VH, Oliveira BP, Rastelli ANS, Bagnato VS. Dental bleaching using violet light alone: clinical case report. Dentistry. 2017; 7(11): 1–4.
- Rastelli ANS, Dias HB, Carrera ET, et al. Violet LED with low concentration carbamide peroxide for dental bleaching: A case report. Photodiagnosis Photodyn Ther. 2018;23: 270–272.
- Zanin F, Panhoca VH, Brugnera AP, Windlin MC, Brugnera A. Dental bleaching. The great leap: the use of light without gel. In: Brugnera A, Namour S, ed. Laser Dentistry: Current Clinical Applications. Irvine, CA: Universal-Publishers 2018: 467.
- Bernardon JK , Sartori N, Ballarin A, et al. Clinical performance of vital bleaching techniques. Oper Dent. 2010;35(1): 3–10.
- Machado LS, de Oliveira FG, Rocha EP, et al. Clinical trial evaluating color change and tooth sensitivity throughout and following in-office bleaching. Int J Periodontics Restorative Dent. 2013;33(2): 209–215.
- Reis A, Kossatz S, Martins GC, Loguercio AD. Efficacy of and effect on tooth sensitivity of in-office bleaching gel concentrations: a randomized clinical trial. Oper Dent. 2013;38(4): 386–393.
- Mondelli RF, Azevedo JF, Francisconi AC, Almeida CM, Ishikiriama SK. Comparative clinical study of the effectiveness of different dental bleaching methods - two year follow-up. J Appl Oral Sci. 2012;20(4): 435–443.
- Moghadam FV, Majidinia S, Chasteen J, Ghavamnasiri M. The degree of color change, rebound effect and sensitivity of bleached teeth associated with at-home and power bleaching techniques: A randomized clinical trial. Eur J Dent. 2013;7(4): 405–411.
- Kwon SR, Wertz PW. Review of the Mechanism of Tooth Whitening. J Esthet Restor Dent. 2015;27(5): 240–257.
- Joiner A. The bleaching of teeth: a review of the literature. J Dent. 2006;34(7): 412–419.
- Florez FLE, Lins EC, Portero PP, et al. Investigation of Photo-Bleaching through transmittance method in pigmented solution: understanding possible mechanisms and advantages for photo dental whitening. Proc SPIE Lasers in Dentistry XIII. 2007; 6425: 64250Y.
- Rueggeberg FA, Giannini M, Arrais CAG, Price RBT. Light curing in dentistry and clinical implications: a literature review. Braz Oral Res. 2017;31(suppl 1): e61.
- Presoto CD, Bortolatto JF, de Carvalho PP, et al. New Parameter for In-Office Dental Bleaching. Case Rep Dent. 2016;2016: 6034757.
- Camargo SE, Cardoso PE, Valera MC, de Araújo MA, Kojima AN. Penetration of 35% hydrogen peroxide into the pulp chamber in bovine teeth after LED or Nd:YAG laser activation. Eur J Esthet Dent. 2009;4(1): 82–88.
- Matis BA, Hamdan YS, Cochran MA, Eckert GJ. A clinical evaluation of a bleaching agent used with and without reservoirs. Oper Dent. 2002;27(1): 5–11.
- Rosa RE, Mondelli RFL. Comparação clínica entre clareamento com e sem fotoativação. DMC Journal. 2009;5: 14–17.
- Kossatz S, Dalanhol AP, Cunha T, Loguercio A, Reis A. Effect of light activation on tooth sensitivity after in-office bleaching. Oper Dent. 2011;36(3): 251–257.
- Kugel G, Ferreira S, Sharma S, Barker ML, Gerlach RW. Clinical trial assessing light enhancement of in-office tooth whitening. J Esthet Restor Dent. 2009;21(5):336-347.
- Moncada G, Sepúlveda D, Elphick K, et al. Effects of light activation, agent concentration, and tooth thickness on dental sensitivity after bleaching. Oper Dent. 2013;38(5): 467–476.
- Vildósola P, Vera F, Ramírez J, et al. Comparison of Effectiveness and Sensitivity Using Two In-Office Bleaching Protocols for a 6% Hydrogen Peroxide Gel in a Randomized Clinical Trial. Oper Dent. 2017;42(3): 244–252.
- Martins I, Onofre S, Franco N, et al. Effectiveness of In-office Hydrogen Peroxide With Two Different Protocols: A Two-center Randomized Clinical Trial. Oper Dent. 2018;43(4): 353–361.
- Baik JW, Rueggeberg FA, Liewehr FR. Effect of light-enhanced bleaching on in vitro surface and intrapulpal temperature rise. J Esthet Restor Dent. 2001;13(6): 370–378.
- Soares DG, Sacono NT, Ribeiro AP, et al. Responses of dental pulp cells to a less invasive bleaching technique applied to adhesive-restored teeth. J Adhes Dent. 2015;17(2): 155–161.
- Lima SNL, Ribeiro IS, Grisotto MA, et al. Evaluation of several clinical parameters after bleaching with hydrogen peroxide at different concentrations: A randomized clinical trial. J Dent. 2018;68: 91–97.
- Cavalli V, Silva BG, Berger SB, et al. Effect of Adhesive Restoration and Bleaching Technique on the Concentration of Hydrogen Peroxide In the Pulp Chamber. Oper Dent. 2017;42(2): E44–E54.
- Carrasco TG, Carrasco-Guerisoli LD, Froner IC. In vitro study of the pulp chamber temperature rise during light-activated bleaching. J Appl Oral Sci. 2008;16(5): 355–359.
- Hahn P, Schondelmaier N, Wolkewitz M, Altenburger MJ, Polydorou O. Efficacy of tooth bleaching with and without light activation and its effect on the pulp temperature: An in vitro study. Odontology. 2013;101(1): 67–74.



