Home / Journal / Physical Medicine and Rehabilitation
Incremental Step Test Results are related to the Six-Minute Walk Distance in Adults with Chronic Obstructive Pulmonary Disease: An Experimental Study
COPD exercise testing six-minute walk test step test field exercise test pulmonary rehabilitation
Meredith King, Sally L. Wootton, Robert Ong, Zoe J. McKeough, and Sarah Dennis
DOI: 10.31532/PhysMedRehabil.2.1.004 07 Apr 2023
Abstract
Background: The incremental step test (IST) could potentially be used to prescribe exercise training in people with COPD. Objective: To examine the relationship between IST total step count (ISTC) and 6MWT distance (6MWD) to determine whether an appropriate walking training prescription can be inferred from the ISTC. Methods: People with COPD were recruited after a PR assessment (including two 6MWTs) and performed one IST. Pearson’s correlation coefficient (r) assessed the relationship between ISTC, 6MWD and other independent variables. An estimated 6MWD equation from ISTC was derived through stepwise linear regression analysis and Bland Altman plots determined agreement between predicted 6MWD based on ISTC and actual 6MWD. Results: Thirty participants (mean [SD] age 74 [7] and FEV1 58 [21] % predicted) completed testing. Mean [SD] ISTC and 6MWD was 86 (40) and 462 (94) metres respectively. A strong positive correlation was found between ISTC and 6MWD (r = 0.82, p<0.001). ISTC and height (r = 0.32, p <0.001) and age (r = 0.22, p <0.003) were weakly associated. The estimated 6MWD equation from the stepwise regression was 6MWD (m) = 1.92 (ISTC) + 296.7. Conclusion: The IST could estimate 6MWD in people with COPD as the tests are strongly correlated.
Keywords
COPD; exercise testing; six-minute walk test; step test; field exercise test; pulmonary rehabilitation
Introduction
In the current climate of COVID-19 there has been an increasing interest in alternative measures of exercise capacity in people with COPD, particularly those that can be performed with minimal space requirements and outside hospital venues for the vulnerable patient population referred to pulmonary rehabilitation (PR) programs.1 Step tests may be a promising alternative to walk tests with the incremental step test (IST) being reproducible and resulting in maximal cardiorespiratory and metabolic responses compared to a cardiopulmonary exercise test (CPET) in people with COPD.2–4 Recently the modified incremental step test (MIST) has been shown to be a reliable measure that can be used to accurately prescribe exercise training with the mode of training being stepping and is responsive to stepping training.5 Walking training is a commonly prescribed, effective mode of exercise training in people with COPD and is normally commenced at a percentage of peak walk speed achieved following a functional walk test such as the 6MWT.6 No previous study has explored the possibility of prescribing walking training following an incremental step test.
This study therefore aimed to: i) examine the relationship between total step count achieved during an IST (ISTC) and distance walked during a 6MWT and ii) compare the cardiorespiratory responses during the IST and 6MWT. We suggest that if there was a strong relationship and agreement between the IST and 6MWT with similar cardiorespiratory responses it would be appropriate to derive an equation to estimate 6MWD following an IST which would allow clinicians to estimate initial walk training prescription in people with COPD.
Methods
PARTICIPANTS
This study was a prospective, multi-centered, measurement study. A convenience sample of participants were recruited following baseline assessment which included the completion of two 6MWTs performed according to standard procedures from four outpatient PR programs in Sydney, Australia. Participants were included in the study if they had a medical diagnosis of mild, moderate or severe COPD according to the GOLD spirometric classification (forced expiratory volume in one second [FEV1] / forced vital capacity FVC] of < 0.7 and FEV1 < 80% -30% predicted) and were in a stable clinical condition. Participants were excluded if they had any of the following: decompensated heart failure (increased dyspnoea, leg/feet swelling, and/or fatigue for more than two days), other comorbidities that prevented them from performing the stepping motion safely, oxygen saturation (SpO2) of <88% on room air at rest, cognitive impairment or insufficient levels of spoken English to understand the test instructions.7,8 Participants were also excluded if their 6MWT had been completed more than four weeks prior to the IST testing date. Written, informed consent was obtained from all participants. The study was approved by the Northern Sydney Local Health District ethics committee (LNR/17/HAWKE/2).
PARTICIPANTS
Incremental step test
Each participant completed an externally paced IST. It was deemed necessary only to perform one IST based on the work by Dal Corso et al. (2013) previously demonstrating that the IST is highly reproducible. The IST requires participants to step up and down on a 20 cm high step (40 cm width, 60 cm depth) with an initial stepping rate of 10 steps/min. Step rate increased by one-step per minute every 30 seconds until it could no longer be tolerated.3,9 This was a modification of the IST protocol used by de Andrade et al (2012) where the step rate increased by one step every 30 seconds, in order to reduce the risk of rapidly increasing step rate causing early cessation of the test. Participants were not permitted to hold a rail during the test to ensure the respiratory accessory muscles were not braced during the test. The test was timed by an independent assessor with the end test time recorded. The primary outcome measure of the test was the ISTC and was determined by converting the end test time into steps by rounding down to the closest 30 second interval.
Six-minute walk test
Each participant’s 6MWT result (best of two tests) was recorded for comparison with measures from the IST. The 6MWT track length varied according to site with all tracks being between 30 to 40 metres. Participants performed both 6MWTs on the same track either on the same day separated by a 30-minute rest period or within seven days. The distance achieved in the test was compared to normative data.10
Cardiorespiratory response
During both the IST and 6MWT, oxygen saturation (SpO2) and heart rate (HR) were continuously monitored (Pulse oximeter; Masimo Rad 5, Masimo Corporation, Irvine, CA, USA or Novametric, Respironics, Murrysville, PA, USA) and recorded each minute. If SpO2 dropped below 80% during testing, the IST was terminated as per the recommendations for other incremental field exercise tests in this population.7 If SpO2 fell below 80% in the 6MWT, a rest was imposed until SpO2 increased to ≥ 90%. Dyspnoea was assessed before and at the end of each exercise test using the modified 0-10 point category-ratio scale.11
SAMPLE SIZE
The sample size was calculated to detect a correlation of at least 0.5 between the ISTC and the 6MWD. With a bidirectional alpha of 0.05 and a power of 80%, 29 subjects was considered a sufficient sample. This was based on the study by de Andrade et al (2012) where they found a correlation of 0.6 between the Chester step test and the IST, from a sample size of 32 participants.3
DATA ANALYSIS
Analysis was performed using SPSS (IBM Corp. Released 2013. IBM SPSS Statistics for Macintosh, Version 27.0. Armonk, NY: IBM Corp). The relationship between IST total step, 6MWD and other independent variables (gender, age, height [metres] and weight [kilograms]) were assessed using Pearson’s correlation coefficient (r) for continuous variable and Spearman’s Rho for categorical variables. Stepwise multiple regression was performed using ISTC, age, height (m), weight (kg) and gender as independent variables and 6MWD as the dependent variable was completed to derive an equation to estimate 6MWD. Bland Altman plots were used to determine agreement between predicted 6MWD from the derived equation and actual 6MWD achieved in the 6MWT. Cardiorespiratory responses during the IST and the 6MWT (Nadir SpO2, HR max and end test dyspnoea) were compared using unpaired t-tests.
Results
Baseline characteristics are presented in Table 1. Between February 2017 and February 2018 30 participants were recruited, 60% were male with a mean age of 75 years (SD 7) and most were ex-smokers. Severity of airflow obstruction was classified according to the GOLD stages and were derived from each participant’s most recent pulmonary function test results, with the majority of participants classified as GOLD Stage II and GOLD Stage III.8
Table 1. Participant Characteristics
Characteristic |
n = 30 |
Gender (male) n(%) |
18 (60%) |
Mean age in years |
75 (7) |
Height [cm] |
166 (9) |
Weight [kg] |
72 (15) |
BMI [kg/m2] |
30.1 (22.9) |
FEV1 [L] |
1.5 (0.6) |
FEV1 [% predicted] |
59 (21) |
FEV1 / FVC |
0.5 (0.1) |
GOLD Stage GOLD I (%) GOLD II (%) GOLD III (%) |
7%40%53% |
Smoking history Ex-smoker (%) Never smoked (%) |
946 |
Co-morbidities Cardiac disease (%) Neurological condition (%) Metabolic condition (%) Musculoskeletal condition (%) Circulatory condition (%) History of cancer (%) Mental illness (%) Renal disease (%) Gastro oesophageal reflux disorder (%) Obstructive sleep apnoea (%) |
30 15 10 70 60 15 10 5 5 5 |
Data presented as mean (SD) unless otherwise stated. BMI: body mass index; cm: centimetres; FEV1: forced expiratory volume in 1 second; FVC: forced vital capacity; GOLD: the global initiative for obstructive lung disease; kg: kilograms; kg/m2: kilograms per metre squared; L: litre; m: metres; yr: years.
Average 6MWD was 462 m (SD 94) being 76% (SD 15) of predicted walk distance.10 ISTC was 109 (SD 61). Cardiopulmonary responses and number of participants completing each stage of the IST are presented in Table 2.
Table 2. Number of participants that completed each time point, absolute and cumulative step counts, and cardiopulmonary responses.
Time[min] |
IST StepCount |
Mean (SD) HR[beats/min] |
Mean (SD) SpO2[%] |
N |
|
0:00 |
0 |
0 |
80 (10) |
95 (2) |
30 |
0:30 |
5 |
5 |
30 |
||
1:00 |
6 |
11 |
94 (9) |
93 (3) |
30 |
1:30 |
6 |
17 |
30 |
||
2:00 |
7 |
24 |
99 (13) |
92 (4) |
30 |
2:30 |
7 |
31 |
29 |
||
3:00 |
8 |
39 |
105 (13) |
92 (6) |
28 |
3:30 |
8 |
47 |
28 |
||
4:00 |
9 |
56 |
108 (15) |
91 (3) |
23 |
4:30 |
9 |
65 |
19 |
||
5:00 |
10 |
75 |
109 (15) |
91 (4) |
19 |
5:30 |
10 |
85 |
15 |
||
6:00 |
11 |
96 |
101 (33) |
85 (25) |
14 |
6:30 |
11 |
107 |
7 |
||
7:00 |
12 |
119 |
103 (11) |
92 (2) |
4 |
7:30 |
12 |
131 |
5 |
||
8:00 |
13 |
144 |
109 (9) |
92 (2) |
5 |
8:30 |
13 |
157 |
3 |
||
9:00 |
14 |
171 |
115 |
90 |
1 |
9:30 |
14 |
185 |
127 |
91 |
1 |
There was a strong correlation between the 6MWD and ISTC (r = 0.82, p <0.001) (Figure 1), a weak association between ISTC and height ((r = 0.32, p <0.001) and age (r = 0.22, p <0.003) and no association with weight (r = 0.14, p <0.003), gender (r = -0.12, p <0.001) or FEV1 (r = 0.14, p <0.001). All independent variables were excluded from the stepwise multiple regression such that estimated 6MWD could be derived using the ISTC by the following equation: Estimated 6MWD (m) from IST = 1.92 (IST total step count) + 296.7. Bland Altman plots demonstrated good agreement with minimal bias between the actual 6MWD and the estimated 6MWD derived from the equation (Figure 2) with the mean difference (± limits of agreement) being 0.21 (± 107) metres, which was not significant (p = 0.075).
Cardiorespiratory responses for HR, SpO2 and dyspnoea between the 6MWT and IST were similar with nadir SpO2 (mean, SD) being 91 (5) % vs 90 (5)%, (p=0.3), HR max 113 vs 116 (p=0.3), end test dyspnoea using the 0-10 category ratio scale 3.07 (0.98) vs 3.52 (1.39) (p=0.15) respectively.12,13
Figure 1. Scatter plot with regression line illustrating the association between 6MWD and IST total step count. 6MWD: six-minute walk distance; IST: incremental step test.
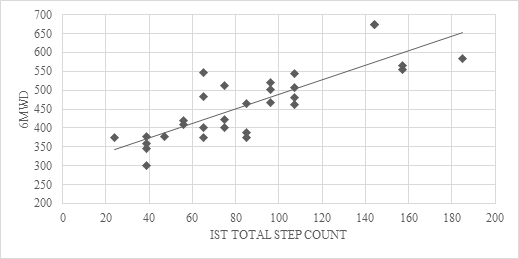
Figure 2. Bland Altman plot of mean 6MWD and predicted 6MWD from IST total step count.
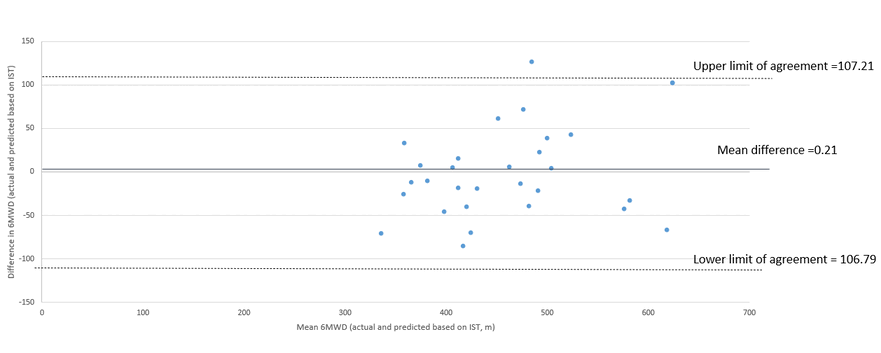
Discussion
This study is the first to assess the relationship between the 6MWT and the IST in people with COPD finding a strong relationship between ISTC and 6MWD. Similar cardiorespiratory responses during both exercise tests were demonstrated and therefore an equation to estimate 6MWD in people with COPD, that would allow prescription of walking training, from the results of the IST was derived (Estimated 6MWD (m) from IST = 1.92 (IST total step count) + 296.7). The IST has been shown previously to elicit similar cardiorespiratory responses to a CPET in people with COPD, pulmonary hypertension, and interstitial lung disease with the IST demonstrating higher levels of oxygen desaturation than CPET in these populations.2,3,12
This study has demonstrated that the IST also elicits similar cardiorespiratory responses to a 6MWT, which is important as the performance of an IST would provide similar information in a way that requires less space.
While there are numerous alternative exercise tests available for use in COPD, in order for a test to be used clinically in a similar way to the 6MWT it needs to be feasible for the majority of people attending PR.1 Previous studies have noted that some participants are unable to complete step tests due to balance or difficulty maintaining the speed.13 While other IST studies have had a faster rate of stepping increase, the study participants were also significantly younger than our population.3,12 In other step tests, the larger incremental step rate increase has been suggested to increase the perception of intensity each time the rate changes which can lead to early cessation of the test and shorter total test time which would limit the true cardiopulmonary response to the test.13 The rate of stepping increase in the current study was slower than other studies with the aim of making the test more achievable for the PR population.2,3,12 All recruited participants were able to complete at least two minutes of the test and the participant demographics were similar to typical PR populations which demonstrates that the IST could be feasible for most people with COPD attending PR programs.6 Previous studies have found similar levels of peak oxygen consumption between step tests and CPET as well as 6MWTs and CPET in COPD indicating that the IST and 6MWT are more than sub-maximal tests in some participants.4,5,14 In the current study, the cardiorespiratory responses in the IST were comparable to the 6MWT., Mean levels of dyspnoea for both tests was three on the modified 0–10 point category-ratio scale which is higher than the level shown to correlate with at least 70% V02 peak in a study looking at another step test in people with COPD.5 This demonstrated that the IST sufficiently challenged exercise capacity in a similar way to a 6MWT. While it has been hypothesised that stepping may be more intense than field-based walking tests due to the vertical displacement in a step test, our study shows that the responses were similar despite the difference in activity performed.15 Our study also asked participants to not hold onto anything during the IST to ensure the respiratory accessory muscles were not braced which is different to other IST protocols.2,3
The equation to estimate 6MWD following the IST was derived as a strong relationship and agreement between the two measures was found. Although the limits of agreement were large (Figure 2), they were non-significant which means we can assume there was no proportional bias. While there are limitations to this analysis in a small sample size, this provides a potential for future research to test the equation in larger samples to ensure generalizability for clinical use and to confirm that other dependent variables such as age, height, weight and gender remain only weakly associated with ISTC. While the IST has already been shown to be able to prescribe stepping training, if the IST can be used to appropriately prescribe intensity of other modes of aerobic training (treadmill or ground walking, cycle ergometers) intensity in a similar way to 6MWT, it would prove to be a useful alternative test in PR programs.17,18 As recently there have been concerns around exercise testing in shared clinical spaces due to the potential risk of aerosolisation with exercise and the mandatory use of masks during exercise testing required in public spaces as required by hospitals finding versatile tests that can be completed safely by people with COPD is increasingly important. Given the IST has been shown to be reliable in home-based settings previously5 and our study demonstrates that the IST is strongly associated with the 6MWT, this would allow the IST to be used in situations where a 6MWT may be less feasible to both identify patients that need further monitoring during exercise as well as prescription of effective walking training.16
There are some limitations to this study. Firstly, assessor bias could be a factor study the IST as the participant continues the test until no longer tolerated (e.g. participant choses to stop), or they are unable to maintain the given step rate for longer than 15 seconds with this latter end test criteria relying heavily on the assessor’s judgment. With the inclusion of additional tasks such as oxygen and heart rate monitoring, attempting to track time and synchronicity of the participant’s steps with the externally paced step rate could be challenging for an inexperienced clinician. Similarly, total step count was rounded to the nearest 30 seconds as it was not possible for the assessor to count the steps while monitoring stepping rate and cardiorespiratory response.
It is important to also consider the use of a convenience sample and the inclusion criteria for this study that may have resulted in selection bias. Participants were excluded if they could not speak English along with those who were unable to perform the step-up movement such as those with other comorbidities like neurological or musculoskeletal impairments without holding onto something. Participant who had low resting oxygen saturation or those that required supplemental oxygen during exercise were also excluded and, therefore, our results cannot be applied to those patient groups. A previous study reported that a high number of people (up to a third of participants) were unable to safely complete the MIST whereas all participants in our study were able to perform the IST for at least two minutes with no adverse events reported and this elicited dyspnoea in all but one participant.5 While this may also represent our exclusion of participants who couldn’t complete the stepping motion safely at baseline, earlier literature using similar exclusion criteria but a faster step rate also found a higher rate of participants stopping the test within the first few minutes.3 This finding suggests that a modified version of the IST with a slower rate of stepping increase may be more acceptable to patients and may be feasible to perform as part of a standard PR assessment.
In this study, we did not have portable gas analysis equipment available for monitoring of oxygen consumption during the exercise tests and were, therefore, unable to compare our responses with findings found in other research examining step tests.5 While other studies appear to indicate that incremental step tests do challenge people with COPD in similar ways to other common field-exercise tests, our decision to use a slower rate of stepping increase may affect the level of oxygen consumption required to do the test.1,5
Further research could investigate the use of the IST in comparison to other commonly used tests such as the incremental shuttle walk tests or incremental cycle testing and whether the ISTC could be used to directly prescribe exercise programs like walking training without being converted back to a 6MWD or other measure.
Conclusion
This study established a strong correlation between ISTC with 6MWD in people with COPD and that the IST could be used to estimate 6MWD in people. The IST may be a possible alternative for assessment of exercise capacity in individuals with COPD in primary and community settings or where space is limited in order to determine appropriate exercise prescription.
Acknowledgements
We would like to thank all the staff in the Chronic Disease Community Rehabilitation Service in Northern Sydney Local Health District for their assistance with this study and to our participants for taking part.
References
- Holland AE, Malaguti C, Hoffman M, et al. Home-based or remote exercise testing in chronic respiratory disease, during the COVID-19 pandemic and beyond: A rapid review. Chronic Respir Disease. 2020; 17: 1–18..
- Dal Corso S, Duarte SR, Neder JA, et al. A step test to assess exercise-related oxygen desaturation in interstitial lung disease. Europ Respir J. 2007; 29: 330–336.
- de Andrade CH, de Camargo AA, de Castro BP, et al. Comparison of cardiopulmonary responses during 2 incremental step tests in subjects with COPD. Respir care. 2012; 57:1920–1926..
- Dal Corso S, de Camargo AA, Izbicki M, et al. A symptom-limited incremental step test determines maximum physiological responses in patients with chronic obstructive pulmonary disease. Respir Med. 2013; 107: 1993–1999.
- Burge AT, Rodrigues JC Jr, Abramson MJ, et al. Application of the Modified Incremental Step Test for Pulmonary Rehabilitation. Phys Therapy. 2021; 101:1–9.
- Wootton SL, Ng LW, McKeough ZJ, et al. Ground-based walking training improves quality of life and exercise capacity in COPD. Europ Respir J. 2014; 44:885–894.
- Holland AE, Spruit MA, Troosters T, et al. An official European Respiratory Society/American Thoracic Society technical standard: field walking tests in chronic respiratory disease. Europ Respir J. 2014; 44:1428-46.
- Global Initiative for Chronic Obstructive Lung Disease. Global strategy for the diagnosis, management, and prevention of COPD. 2014; Available from: www.goldcopd.org
- Dal Corso S, Oliveir AN, Izbicki M, et al. Symptom-Limited Incremental Step Test in COPD Patients: Reproducibility and Validity Compared to Incremental Cycle Ergometry. A107 Adding to the science of pulmonary rehabilitation. American Thoracic Society International Conference. 2009; Abstracts: A2364.
- Borg G. Psychophysical bases of perceived exertion. Med Sci Sports Exe. 1982; 14: 377–381.
- Jenkins S, Cecins N, Camarri B, et al. Regression equations to predict 6-minute walk distance in middle-aged and elderly adults. Physiother Theory Pract. 2009; 25: 516–522.
- Vieira EB, Ota-Arakaki JS, Dal Corso S, et al. Incremental step test in patients with pulmonary hypertension. Respir Physiol Neurobiol. 2020; 271: 103307.
- Bohannon RW, Bubela DJ, Wang YC, et al. Six-Minute Walk Test Vs. Three-Minute Step Test for Measuring Functional Endurance. J Strength Cond Res. 2015; 29: 3240–3244.
- Hill K, Dolmage TE, Woon L, et al. Comparing peak and submaximal cardiorespiratory responses during field walking tests with incremental cycle ergometry in COPD. Respirol. 2012; 17: 278–284.
- de Camargo AA, Justino T, de Andrade HS, et al. Chester Step Test in Patients With COPD: Reliability and Correlation With Pulmonary Function Test Results. Respir care. 2011; 56: 995–1001.
- Gemicioğlu B, Börekçi Ş, Dilektaşlı AG, et al. Turkish Thoracic Society Experts Consensus Report: Recommendations for Pulmonary Function Tests During and After COVID 19 Pandemic. Turk. Thorac J. 2020; 21:193–200.
- Zainuldin R, Mackey MG, Alison, JA. Prescription of walking exercise intensity from the 6-minute walk test in people with chronic obstructive pulmonary disease. J Cardiopulm Rehabil Prev. 2015; 235: 65–69.
- Hill, K, Jenkins SC, Cecins N, et al. Estimating Maximum Work Rate During Incremental Cycle Ergometry Testing from Six-Minute Walk Distance in Patients with Chronic Obstructive Pulmonary Disease. Arch Phys Med Rehabil. 2008; 89: 1782–1787.



