Home / Journal / Physical Medicine and Rehabilitation
Comprehensive Preoperative Pulmonary Rehabilitation Including Intensive Nutritional Support Reduces the Postoperative Morbidity Rate of Sarcopenia-Related Patients with Lung Cancer
Lung cancer Postoperative complication Preoperative pulmonary rehabilitation Sarcopenia
Hiroaki Harada, Miho Takahama, Junichi Nakao, Yoshinori Yamashita, and Kiyomi Taniyama
DOI: 10.31532/PhysMedRehabil.2.1.001 06 Apr 2018
Abstract
Since surgical resection is the treatment of choice for localized lung cancer, it is important to develop an effective strategy to reduce the risk of postoperative complications caused by poor preoperative conditions. We prospectively implemented a comprehensive preoperative pulmonary rehabilitation (CHPPR) program that includes intensive nutritional support with branched-chain amino acids and herbal medicine supplementation concomitant with potential high-intensity physical therapy through an interdisciplinary team approach. This study aimed to evaluate whether CHPPR is beneficial for elderly, low body weight (percentage ideal body weight <90%) patients scheduled to undergo lung surgery. Between 2006 and 2015, 171 patients aged >70 years underwent standard lobectomy for lung cancers. Of these, 12 patients with a low body weight (sarcopenia-related, Group A) and 62 patients without a low body weight (sarcopenia-unrelated, Group B) underwent surgery after CHPPR. Twenty-four patients with a low body weight (sarcopenia-related, Group C) and 73 patients without a low body weight (sarcopenia-unrelated, Group D) refused CHPPR. The postoperative morbidity rates of patients in Groups A, B, C, and D were 17%, 16%, 63%, and 21%, respectively. Of the patients in the sarcopenia-related groups (Groups A and C), those who participated in the CHPPR program (Group A) had a significantly lower morbidity rate than those who did not participate in the CHPPR program (Group C) (P = 0.014). The CHPPR program is beneficial in reducing the postoperative morbidity rate of sarcopenia-related patients scheduled to undergo pulmonary resection.
Keywords
Lung cancer, Postoperative complication, Preoperative pulmonary rehabilitation, Sarcopenia
Introduction
Since the standard treatment of localized lung cancer is surgical resection, developing an effective intervention to reduce the risk of postoperative complications caused by insufficient preoperative preparation is important. Therefore, improving general and physical conditioning preoperatively should be considered essential for patients undergoing lung surgery.1,2 Over the past few decades, improvements in perioperative management, including physical therapy, have contributed to reduced complication and mortality rates after lung resection. 3,4 Pulmonary rehabilitation has been shown to be a beneficial intervention for improving pulmonary conditions. Although the duration of a standard program has generally been 6 to 12 weeks,5,6 a recent study has demonstrated the benefit of short-term preoperative rehabilitation in patients undergoing pulmonary resection for non-small cell lung cancer7. However, its effect on reducing morbidity after pulmonary resection has not been clearly elucidated.8 Thus, we have prospectively implemented a comprehensive preoperative pulmonary rehabilitation (CHPPR) program that includes intensive nutritional support with branched-chain amino acids (BCAAs) and herbal medicine supplementation concomitant with standard physical exercise through an interdisciplinary team approach.
Sarcopenia is a syndrome characterized by progressive and generalized loss of skeletal muscle mass and strength.9 Within the medical community, sarcopenia is recognized as a serious condition that is often associated with poor physical mobility and negative clinical outcomes among older adults.10 Peng et al. reported that sarcopenia was associated with an increased risk of major postoperative complications after liver resection for colorectal liver metastases11, and Lieffers et al. reported that sarcopenia was a predictive factor for postoperative infections and delayed recovery from colorectal cancer resection12. However, few studies have focused on the effects of preoperative pulmonary rehabilitation in patients with sarcopenia scheduled to undergo pulmonary resection.
We have demonstrated the beneficial effects of our CHPPR program. 13,14 However, little attention has been given to the association between sarcopenia and postoperative complications. A main component of our CHPPR program is intensive nutritional support with BCAAs that serve as essential substrates and important regulators of protein synthesis in muscle tissue. However, the effect of BCAA supplementation on the clinical outcomes of patients with sarcopenia and lung cancer patients remains unclear. Thus, the main objective of the present study was to determine the efficacy of our specific CHPPR program for reducing morbidity after lung resection, especially in elderly (>70 years of age), low body weight (percentage ideal body weight <90%) patients.
Materials and Methods
Study population and CHPPR protocol Since June 2009, we have prospectively implemented a CHPPR program that includes three main components: (1) Multiple sessions of potential high-intensity physical therapy and exercise (at least twice a week for 2 to 5 weeks), guided and assessed by physical therapists; (2) intensive nutritional support with BCAAs (6.4 g/day) (Hepas SecondTM; Clinico Co., Tokyo, Japan or AminofeelTM; Terumo Co., Tokyo, Japan) and herbal medicine supplementation (HochuekkitoTM; Tsumura Co., Tokyo, Japan), guided and assessed by registered dieticians; and (3) an interdisciplinary team approach (Figure 1).14 The protocol of this study was approved by Institutional Review Board Ethics Committee and informed consent was obtained from all enrolled patients. Team conferences on an equal basis with all involved specialists, including doctors, physical therapists, dieticians, nurses, physiology laboratory technicians, and a clinical research coordinator, were routinely held to discuss efficient strategies for improving each patient’s status.
Figure 1. Three fundamental components of the CHPPR protocol
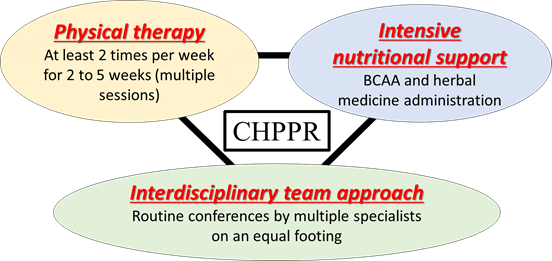
CHPPR program includes potential high-intensity physical therapy concomitant with intensive nutritional support with BCAAs and herbal medicine supplementation through an interdisciplinary team approach. Abbreviations: BCAA, branched-chain amino acid; CHPPR, comprehensive preoperative pulmonary rehabilitation.
Patients who met at least one of the following criteria were recommended to participate in the CHPPR program: age ≥70 years, percentage vital capacity <80%, forced expiratory volume in one second (FEV1)/forced VC <70%, and percentage ideal body weight <90%. The preoperative evaluation of patients did not routinely include a 6-minute walking or stair climbing test.
Between 2006 and 2015, 171 patients aged >70 years underwent standard lobectomy for lung cancer at our hospital. Twelve patients with a low body weight (sarcopenia-related, Group A) and 62 patients without a low body weight (sarcopenia-unrelated, Group B) underwent surgery after CHPPR. Twenty-four patients with a low body weight (sarcopenia-related, Group C) and 73 patients without a low body weight (sarcopenia-unrelated, Group D) refused to participate in the CHPPR program. The assignment of patients was mainly based on their preference. Therefore, this was not a randomized study. Eight of the 171 patients included in this study had a performance status of ≥2, mainly due to dementia. Three of the 8 patients participated in the CHPPR program and completed it with the assistance of their family.
Assessment of postoperative outcome The postoperative outcomes of the 4 groups were assessed. Morbidity was defined as the ratio of patients who developed postoperative complications of Grade ≥2 according to the Clavien-Dindo classification system. Changes in pulmonary function between pre and post CHPPR were evaluated.
Statistical analyses Comparisons were performed using JMP software for Windows (version 9.02; SAS Institute, NC, USA). Results are expressed as means ± standard errors. Differences in characteristics and postoperative complication rates (morbidity) between the CHPPR and non-CHPPR groups were determined using the Mann-Whitney U test or Fisher’s exact test. Univariate and multivariate logistic regression analysis of morbidity was also conducted. Differences were considered statistically significant at P < 0.05.
Results
Characteristics and postoperative outcomes Table 1 shows the patient characteristics and perioperative conditions, including preoperative risk score of Estimation of Physiological Ability and Surgical Stress,15 of the 4 groups. Although there was no significant difference in stage distribution (P = 0.927), statistically significant differences were observed in the operative time (P < 0.001) and amount of blood loss (P = 0.001) between the 4 groups. The postoperative morbidity rates were 17%, 16%, 63%, and 21% for Groups A, B, C, and D, respectively (Figure 2). For patients who participated in the CHPPR program (Groups A and B), there was no difference in the morbidity rate between sarcopenia-related (Group A) and sarcopenia-unrelated (Group B) patients (P = 1.000). For patients who did not participate in the CHPPR program (Groups C and D), there was a significant difference in the morbidity rate, with patients in Group C (sarcopenia-related) developing postoperative morbidity significantly more frequently than patients in Group D (sarcopenia-unrelated) (P < 0.001). One patient in Group B and 4 patients in Group C died from postoperative complications. The cause of death in the patient in Group B was empyema. Three patients in Group C died of acute exacerbation of interstitial pneumonia. The other patient in Group C died suddenly from an unknown cause.
Table 1. Patient characteristics
|
Characteristic |
Group A |
Group B |
Group C |
Group D |
P- value |
|
n = 12 |
n = 62 |
n = 24 |
n = 73 |
||
|
CHPPR |
Yes |
Yes |
No |
No |
– |
|
Sarcopenia-related |
Yes |
No |
Yes |
No |
– |
|
Age (years), mean ± SE |
75.5 ± 1.1 |
76.2 ± 1.6 |
75.5 ± 0.8 |
75.5 ± 0.5 |
0.788 |
|
Sex (female/male) |
5/7 |
22/40 |
5/19 |
31/42 |
0.283 |
|
%VC, mean ± SE |
105.0 ± 5.3 |
99.2 ± 2.3 |
92.7 ± 3.7 |
100.3 ± 2.1 |
0.214 |
|
FEV1.0%, mean ± SE |
78.2 ± 2.8 |
74.4 ± 1.2 |
75.8 ± 2.0 |
74.4 ± 1.1 |
0.589 |
|
Approach (VATS/open) |
11/1 |
53/9 |
17/7 |
57/16 |
0.504 |
|
Operative time (mins), mean ± SE |
222.1 ± 26.5 |
219.7 ± 11.7 |
318.5 ± 18.7 |
285.0 ± 10.7 |
<0.001 |
|
Blood loss (g), mean ± SE |
174.2 ± 96.2 |
159.9 ± 42.3 |
479.2 ± 68.0 |
251.2 ± 39.0 |
0.001 |
|
pStage (IAB/IIAB/III–IV)a |
8/2/2 |
38/14/10 |
18/3/3 |
49/15/9 |
0.927 |
|
Smoking status (never/former or current) |
5/7 |
21/41 |
7/17 |
25/48 |
0.904 |
|
PRS of E-PASS, mean ± SE |
0.476 ± 0.051 |
0.488 ± 0.042 |
0.455 ± 0.036 |
0.475 ± 0.038 |
0.825 |
a Tumor-node-metastasis classification (7th edition)
Abbreviations: CHPPR, comprehensive preoperative pulmonary rehabilitation; E-PASS, Estimation of Physiological Ability and Surgical Stress; FEV1.0%, forced expiratory volume in one second/forced Vital capacity; PRS, preoperative risk score; pStage, pathological stage; SE, standard error; VATS, video-assisted thoracic surgery; %VC, percentage vital capacity.
Figure 2. Morbidity rates after standard lobectomy in patients with and without sarcopenia
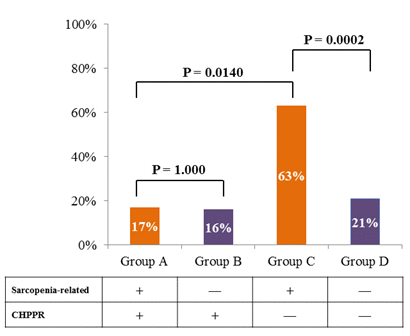
The postoperative morbidity rates of patients in Groups A, B, C, and D were 17%, 16%, 63%, and 21%, respectively. Abbreviations: CHPPR, comprehensive preoperative pulmonary rehabilitation.
Efficacy of CHPPR for sarcopenia-related patients Of the patients in the sarcopenia-related groups (Groups A and C), those who participated in the CHPPR program (Group A) had a significantly lower morbidity rate than those who did not participate in the CHPPR program (Group C) (P = 0.014). In addition, for patients in the sarcopenia-related groups (Groups A and C), univariate logistic regression analysis of risk factors for morbidity showed that age, operative approach, operative time, amount of blood loss, and CHPPR participation were statistically significant factors associated with morbidity (P = 0.046, P = 0.007, P = 0.001, P = 0.004, and P = 0.007, respectively) (Table 2). Multivariate logistic regression analysis revealed that age and CHPPR participation were independent significant factors for reducing morbidity rates (P = 0.043 and P = 0.039, respectively) (Table 3). Table 4 shows the differences in types and grades of postoperative complications between Groups A and C. Group C had a higher grade and frequency of postoperative complications than Group A. Changes in percentage vital capacity and forced expiratory volume in one second in Group A were not significantly different before and after CHPPR ( P = 0.078 and P = 0.279, respectively).
Table 2. Univariate logistic regression analysis for postoperative morbidity in patients with sarcopenia
|
Factor |
Odds ratio |
95.0% CI |
P -value |
|
Age (years) |
1.23 |
1.00–1.56 |
0.046 |
|
Sex (male/female) |
2.72 |
0.61–14.88 |
0.194 |
|
%VC |
0.98 |
0.94–1.02 |
0.252 |
|
FEV1.0% |
0.98 |
0.92–1.04 |
0.490 |
|
Approach (VATS/open) |
0.08 |
0.00–0.53 |
0.007 |
|
Operative time (mins) |
1.01 |
1.00–1.03 |
0.001 |
|
Blood loss (g) |
1.00 |
1.00–1.01 |
0.004 |
|
Smoking status (never/former or current) |
2.34 |
0.58–10.92 |
0.234 |
|
CHPPR (yes/no) |
0.12 |
0.02–0.58 |
0.007 |
Abbreviations: CHPPR, comprehensive preoperative pulmonary rehabilitation; CI, confidence interval; FEV1.0%, forced expiratory volume in one second/forced Vital capacity; VATS, video-assisted thoracic surgery; %VC, percentage vital capacity.
Table 3. Multivariate logistic regression analysis for postoperative morbidity in patients with sarcopenia
|
Factor |
Odds ratio |
95.0% CI |
P- value |
|
Age (years) |
1.36 |
1.01–1.96 |
0.043 |
|
Sex (male/female) |
9.52 |
6.85e-7–31.68 |
0.522 |
|
%VC |
1.04 |
0.97–1.12 |
0.304 |
|
FEV1.0% |
1.03 |
0.94–1.15 |
0.510 |
|
Approach (VATS/open) |
0.35 |
0.01–5.99 |
0.472 |
|
Operative time (mins) |
1.00 |
0.98–1.03 |
0.781 |
|
Blood loss (g) |
1.00 |
1.00–1.01 |
0.458 |
|
Smoking status (never/former or current) |
20.2 |
0.01–2332124 |
0.343 |
|
CHPPR (yes/no) |
0.07 |
0.00–0.89 |
0.039 |
Abbreviations: CHPPR, comprehensive preoperative pulmonary rehabilitation; CI, confidence interval; FEV1.0%, forced expiratory volume in one second/forced Vital capacity; VATS, video-assisted thoracic surgery; %VC, percentage vital capacity.
Table 4. Postoperative complications in patients with sarcopenia according to the Clavien-Dindo classification
|
Complication |
Grade(s) |
CHPPR |
Non-CHPPR |
|
(n = 12) |
(n = 24) |
||
|
Respiratory |
2 |
1 (8.3%) |
4 (16.7%) |
|
3–5 |
1 (8.3%) |
6 (25.0%) |
|
|
Cardiovascular |
2 |
0 (0.0%) |
2 (8.3%) |
|
3–5 |
0 (0.0%) |
0 (0.0%) |
|
|
Other |
2 |
0 (0.0%) |
1 (4.2%) |
|
3–5 |
0 (0.0%) |
2 (8.3%) |
|
|
Total |
2 |
1 (8.3%) |
7 (29.2%) |
|
3–5 |
1 (8.3%) |
8 (33.3%) |
Abbreviations: CHPPR, comprehensive preoperative pulmonary rehabilitation.
Discussion
Pulmonary rehabilitation has been recommended as a component of perioperative management to enhance recovery after thoracic surgery. 16 However, the impact of preoperative pulmonary rehabilitation for patients with lung cancer, with special emphasis on postoperative complications, requires further investigation.17 Since patients with malignant disease should undergo surgery without delay, an effective, short-term, preoperative pulmonary rehabilitation program should be adopted. Therefore, comprehensive management strategies for these patients remain an important issue. To establish an enforceable and beneficial short-term preoperative pulmonary rehabilitation program for outpatients, we developed the CHPPR protocol, consisting of potential high-intensity physical therapy, intensive nutritional support with BCAAs and herbal medication, and an interdisciplinary team approach. Although there is a growing body of evidence to suggest that patients with sarcopenia tend to have poorer clinical outcomes,12 the present study demonstrates that a CHPPR program could aid in the reduction of morbidity rates after lung resection in elderly, low body weight patients.
Preoperative nutritional status may be an important predictor of morbidity and mortality in patients undergoing surgery for malignant disease. 18–20 However, effective preoperative nutritional intervention has not yet been elucidated. BCAAs are among the nine essential amino acids for humans. They play an important role in the formation of skeletal muscle because they account for 35% of the essential amino acids in muscle proteins.21 Several studies have demonstrated that glutamine supplementation, which is produced by BCAAs, improves clinical outcomes and function under certain pathological conditions22,23. Recent literature has reported that BCAA supplementation could be beneficial in improving whole-body protein metabolism in patients with chronic obstructive pulmonary disease24. Takata et al. demonstrated the efficacy and safety of BCAA supplementation used in conjunction with cardiac rehabilitation for patients with chronic heart failure25. Furthermore, it is usually difficult to achieve adequate nutritional intake in elderly patients with pulmonary disorders. For maintenance or improvement of appetite, herbal medications, such as HochuekkitoTM, have been recognized as beneficial supplements, and the effects of such medications on chronic obstructive pulmonary disease have also been evaluated in terms of quality of life.26 In consideration of the aforementioned evidence, we adopted BCAA and herbal medicine administration as intensive nutritional support within our CHPPR program. Although the main aim of intensive nutritional support with BCAA and herbal medicine administration is to support high-intensity physical exercise, the results of the current study demonstrate that preoperative nutritional modification itself may have beneficial effects on postoperative outcomes in patients with sarcopenia-related disease. Previously, changes in hematological nutritional status had been assessed in 17 consecutive patients who had undergone CHPPR, although this included both patients with and without sarcopenia (data not published). Changes in retinol, but not prealbumin, values in blood were statistically significant between pre and post CHPPR (P = 0.022 and P = 0.078, respectively). This suggests that our specific CHPPR protocol has a beneficial nutritional effect despite the relatively short-term program.
Recently, immunonutrition, which is the combination of standard nutritional formulas and immunonutrients, such as glutamine, arginine, and polyunsaturated fatty acids (omega-3), has been widely implemented.27 A growing body of evidence suggests that immunonutrition can reduce infectious postoperative conditions. Therefore, further investigations using various types of nutritional support intervention should be conducted to establish more sophisticated and effective preoperative pulmonary rehabilitation protocols.
Throughout this study, the empowerment of patients and medical staff has been a key factor in our specific CHPPR protocol. The interdisciplinary team approach, which was accomplished through routine conferences on an equal basis with all involved specialists and multiple sessional assessment and guidance for individual patients by multiple specialists, is an integral element for the willingness of not only the patients, but also the team members.
This study has several limitations. First, it was based on data from patients recruited at a single institution. Second, the study cohort was not randomized. Third, the number of patients in our cohort was relatively small. Finally, although evaluating changes in pulmonary function and body weight did not show a statistically significant improvement, various other factors, such as body composition, muscle mass, and length of hospital stay will need to be evaluated to fully elucidate the efficacy of our specific CHPPR protocol. Further investigations using larger sample sizes are warranted to better determine how our CHPPR program contributes to patient outcomes.
Although this was not a randomized controlled study and the sample size was limited, the relatively short-term CHPPR program, which comprised three fundamental components, appeared to have beneficial effects for elderly, low body weight patients scheduled to undergo standard lobectomy for lung cancer. There is growing evidence to suggest that preoperative interventions based on moderate to intense aerobic exercise in patients undergoing lung resection for lung cancer improve functional capacity and reduce postoperative mortality. However, more comprehensive and sophisticated management strategies for patients with lung cancer planning to undergo pulmonary resection need to be investigated.
Conclusion
Our CHPPR protocol comprising several integral components (physical therapy, intensive nutritional support, and an interdisciplinary team approach) appeared to have a beneficial effect on elderly, low body weight patients scheduled to undergo pulmonary resection.
Acknowledgements
We wish to thank the staff at the Institute for Clinical Research, National Hospital Organization Kure Medical Center (Kure, Japan) for their assistance in this study, and Editage (www.editage.jp) for English language editing.
Funding Information
The authors have no support or funding to report.
Conflict of Interest
The authors have no conflicts of interest to disclose.
References
- Jones LW, Peddle CJ, Eves ND, et al. Effects of presurgical exercise training on cardiorespiratory fitness among patients undergoing thoracic surgery for malignant lung lesions. Cancer. 2007; 110: 590–598.
- Cesario A, Ferri L, Galetta D, et al. Pre-operative pulmonary rehabilitation and surgery for lung cancer. Lung Cancer. 2007; 57: 118–119.
- Novoa N, Ballesteros E, Jiménez MF, Aranda JL, Varela G. Chest physiotherapy revisited: evaluation of its influence on the pulmonary morbidity after pulmonary resection. Eur J Cardiothorac Surg. 2011; 40: 130–134.
- Varela G, Ballesteros E, Jiménez MF, Novoa N, Aranda JL. Cost-effectiveness analysis of prophylactic respiratory physiotherapy in pulmonary lobectomy. Eur J Cardiothorac Surg. 2006; 29: 216–220.
- Nici L. Preoperative and postoperative pulmonary rehabilitation in lung cancer patients. Thorac Surg Clin. 2008; 18: 39–43.
- Niewoehner DE. Clinical practice. Outpatient management of severe COPD . N Engl J Med. 2010; 362: 1407–16.
- Benzo R, Wigle D, Novotny P, et al. Preoperative pulmonary rehabilitation before lung cancer resection: results from two randomized studies. Lung Cancer. 2011; 74: 441–445.
- Bradley A, Marshall A, Stonehewer, et al. Pulmonary rehabilitation programme for patients undergoing curative lung cancer surgery. Eur J Cardiothorac Surg. 2013; 44: e266–e271.
- Cruz-Jentoft AJ, Baeyens JP, Bauer JM, et al. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing. 2010; 39: 412–423.
- van Vledder MG, Levolger S, Ayez N, et al. Body composition and outcome in patients undergoing resection of colorectal liver metastases. Br J Surg. 2012; 99: 550–557.
- Peng PD, van Vledder MG, Tsai S, et al. Sarcopenia negatively impacts short-term outcomes in patients undergoing hepatic resection for colorectal liver metastasis. HPB (Oxford). 2011; 13: 439–446.
- Lieffers JR, Bathe OF, Fassbender K, Winget M, Baracos VE. Sarcopenia is associated with postoperative infection and delayed recovery from colorectal cancer resection surgery. Br J Cancer. 2012; 107: 931–936.
- Harada H, Matsuda S, Takahama M, et al. Efficacy of Comprehensive Preoperative Pulmonary Rehabilitation Including Intensive Nutritional Support Through an Interdisciplinary Team Approach. Int J Phys Med Rehabil. 2016; 4: 376.
- Harada H, Yamashita Y, Misumi K, et al. Multidisciplinary team-based approach for comprehensive preoperative pulmonary rehabilitation including intensive nutritional support for lung cancer patients. PLoS One. 2013; 8: e59566.
- Yamashita S, Haga Y, Nemoto E, Nagai S, Ohta M. E-PASS (The Estimation of Physiologic Ability and Surgical Stress) scoring system helps the prediction of postoperative morbidity and mortality in thoracic surgery. Eur Surg Res. 2004; 36: 249–255.
- Jones NL, Edmonds L, Ghosh S, Klein AA. A review of enhanced recovery for thoracic anaesthesia and surgery. Anaesthesia. 2013; 68: 179–189.
- Nagarajan K, Bennett A, Agostini P, Naidu B. Is preoperative physiotherapy/pulmonary rehabilitation beneficial in lung resection patients? Interact Cardiovasc Thorac Surg. 2011; 13: 300–302.
- Gregg JR, Cookson MS, Phillips S, et al. Effect of preoperative nutritional deficiency on mortality after radical cystectomy for bladder cancer. J Urol. 2011; 185: 90–96.
- Morgan TM, Tang D, Stratton KL, et al. Preoperative nutritional status is an important predictor of survival in patients undergoing surgery for renal cell carcinoma. Eur Urol. 2011; 59: 923–928.
- Zemanova M, Novak F, Vitek P, et al. Outcomes of patients with oesophageal cancer treated with preoperative chemoradiotherapy, followed by tumor resection: influence of nutritional factors. J BUON. 2012; 17: 310–316.
- Harper AE, Miller RH, Block KP. Branched-chain amino acid metabolism . Annu Rev Nutr. 1984; 4: 409–454.
- Choudry HA, Pan M, Karinch AM, Souba WW. Branched-chain amino acid-enriched nutritional support in surgical and cancer patients. J Nutr. 2006; 136: 314S–318S.
- Boelens PG, Nijveldt RJ, Houdijk AP, Meijer S, van Leeuwen PA. Glutamine alimentation in catabolic state. J Nutr. 2001; 131: 2569S–2577S.
- Engelen MP, Rutten EP, De Castro CL, Wouters EF, Schols AM, et al. Supplementation of soy protein with branched-chain amino acids alters protein metabolism in healthy elderly and even more in patients with chronic obstructive pulmonary disease. Am J Clin Nutr. 2007; 85: 431–439.
- Takata M, Amiya E, Watanabe M, et al. An exploratory study on the efficacy and safety of a BCAA preparation used in combination with cardiac rehabilitation for patients with chronic heart failure. BMC Cardiovasc Disord. 2017; 17: 205.
- Guo R, Pittler MH, Ernst E. Herbal medicines for the treatment of COPD: a systematic review. Eur Respir J. 2006; 28: 330–338.
- Giger U, Büchler M, Farhadi J, et al. Preoperative immunonutrition suppresses perioperative inflammatory response in patients with major abdominal surgery-a randomized controlled pilot study. Ann Surg Oncol. 2007; 14: 2798–2806.



