Home / Journal / Oral Health and Dental Studies
Pierre Robin Sequence- Manifestation and Case Report
pierre Robin sequence micrognathia retrognathic mandible glossoptosis orthodontic treatment
Eliyahu Mass, Shelly Segal,Yael Arieli, and Uri Zilberman
DOI: 10.31532/OralHealthDentStud.1.1.004 08 Jun 2018
Abstract
A boy with Pierre Robin sequence, an autosomal recessive inherited craniofacial anomaly, defined as suffering from a chronic condition that puts him in the category of children with special needs, received comprehensive dental and orthodontic treatment. The child was diagnosed immediately after birth and suffered from respiratory and feeding problems that required tracheotomy and gastrostomy, and surgical repair of cleft palate. The course of treatments, the complications, and their solutions is described. A multidisciplinary team including pediatric, ENT, general and oral surgeons, speech therapist, pediatric dentist, and orthodontic specialists should be involved in the treatment of PRS children for a relatively better quality of life outcome.
Keywords
Pierre Robin sequence, Micrognathia, Retrognathic mandible, Glossoptosis, Orthodontic treatment
Introduction
According to the Clinical Consensus report on Pierre Robin sequence (PRS), Pierre Robin is comprising of mandibular micrognathia, glossoptosis and airway obstruction, leading to life-threatening obstructive apnea and feeding difficulties during the neonatal period.1 Cleft palate is considered a common and additional feature, but not a perquisite for diagnosis.
The sequence is named after Pierre Robin, whose report was published in 1923 (earlier reports were in 1822). The reported incidence is estimated to be 1:8,500-14,000.2,3 Williams and his colleagues have argued that not every child with a cleft palate and micrognatia is defined as suffering from PRS, but breathing difficulty is a necessary element for the definition4.
The syndrome is defined as a sequence, a collection of anomalies caused by early developmental disorders or mechanical processes. The explanation of the sequence definition rather than a syndrome is based on early mandibular developmental disorder, which leads to abnormal tongue position, followed by a series of events, leading to formation of cleft lip and palate.5
Fourteen different phenotypes of PRS were found, which accentuate the variability of the diagnosis and definition.5 The differences in defining the sequence also cause differences in the prevalence and in reports of related syndromes.5,6
PRS may be identified in more than 40 syndromes. It is difficult to identify it during birth and to distinguish it from other related syndromes.
Clinical manifestations At birth the face of PRS appears prominent. The mandible is small and deflecting backwards. For most clinicians, the diagnosis of micrognathia is largely subjective. The optimal tool to measure mandibular micrognathia during childhood, not only in PRS cases, should be the Jaw Index.7 Glossoptosis is a clinical entity defined as displacement of the tongue base into the oropharynx and hypopharynx. There is no definitive correlation between the degree of micrognathia and severity of glossoptosis.8 Cleft palate may sometimes appear U-shaped, but current publications are contradictory about whether the cleft in PRS is more extensive than the non-PRS cleft palate.9 Clinical signs of respiratory compromise in PRS children include stertor or stridor, labored breathing, diaphoresis, apnea, and restlessness and can be assessed during sleep, in wakefulness and with feeding.10 There are difficulties at the inspiratory phase of strenuous breathing leading to cyanotic seizures and disengagement of the sternum and the ribs. This is especially noticeable when the child is lying on his back.
Although there is no agreement regarding the defect mechanism of breathing and feeding, the classical explanation is the mandibular micrognathia which does not provide sufficient support to the muscles of the tongue. This leads to the dropping of the tongue down and backwards to the lower post pharyngeal space (glossoptosis), blocking the epiglottis. In this position the tongue allows expirium, but prevents inspirium, acting as a ball valve which causes cyanotic attacks and withdrawal of the sternum.5
Feeding disorders in PRS children can be defined as the inability to take in adequate oral feeds efficiently to support normal growth or oral feeding that potentiates airway or respiratory compromise.1 Abnormal maxillary morphology was also described, associated with midface hypoplasia, thereby causing breathing difficulty. Breathing improves with time because the mandible grows faster during the postpartum period and because of the tongue position is improving with growth and neurological development.5
Significant eating disorders and necessary tube feeding is found in 38-62% of children with PRS. This is due to the inadequate control of the tongue. Breast feeding is causing great suffering. When it comes in Isolated Robin Sequence, feeding problems disappear after the age of one year. Growth disorders, which often are associated with the PRS might be related to the severity of breathing problems, feeding problems, or as part of characteristic features of the syndrome.6 Analysis of facial growth during adolescent showed that PRS subjects have smaller cranial base length, shorter maxillary and mandibular lengths, increased palatal and mandibular plane inclinations and more open mandibular flexure. The maxilla and the mandible remained retrusive during adolescent growth and the maxilla become more retrognathic.10
Case Report
N.A. was 7 years, 2 months old, when first referred from the cleft lip and palate forum (a multidisciplinary group at Soroka Medical Center, Beer Sheva), to the Pediatric Dentistry Unit, Barzilai Medical University Center, Ashkelon, Israel. He was the oldest son, with 2 younger brothers, from a family of Bedouin. The reason for his referral was a need for dental treatment of severe carious lesions and dental crowding.
He was born in the 29th gestation week, weighting 1.180 Kg and diagnosed as suffering from Pierre Robin Sequence. During bodily systems screening, the ultra sound examination revealed a small and backwards mandible.
After birth, he has been ventilated and transferred to the NICU (Neonatal Intensive Care Unit), staying there for about 3 months. Twenty days after birth, surgical tracheotomy was performed, due to severe respiratory problems. According to the mother, the respiratory condition improved dramatically after the surgery.
About 3 months after birth a gastrostom has been inserted, because of feeding difficulties. During the first year of life he was hospitalized several times due to fever spurts and breathing difficulties. He underwent surgery to repair the cleft palate immediately after the appendix has been removed at the age of 1 year.
When he was 18 months the respiratory tube has been removed and with the improvement in eating at the age of 2 years, the gastrostom tube was also removed. Ever since, he is treated and monitored by an Ear Nose and Throat doctor and a speech therapist. There has been a hearing loss although he underwent several surgical tubing (ears buttons).
Dental history N.A. had never visited a dental clinic till the age of 7 years. Occasionally, he brushes his teeth with a toothpaste. He eats many sweets and snacks and his drinks are usually sweet carbonated drinks.
Clinical examination Extra oral: Facial asymmetry, especially in the nose area, was observed due to a different size of the nostrils (Figure 1). Submandibular lymph nodes were not detected.
Intra oral: • Soft tissue: a small residual fistula at the site of the soft palate cleft repair, which does not interfere with function. Otherwise, the soft tissues were normal with mild gingivitis.
• Dentition: Early mixed crowded dentition, with skeletal Angle class II and X-bite of the canines; carious lesions and poor oral hygiene. No hypodontia was found.
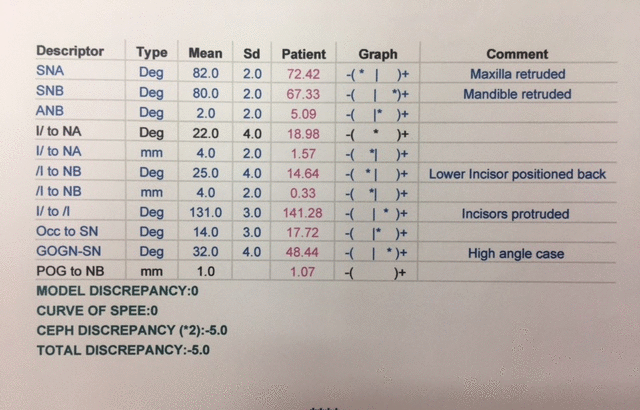
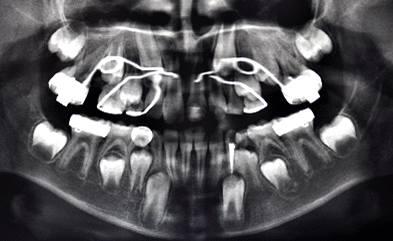
• Special Findings: small retrognathic mandible, retruded maxilla and retruded upper incisors, lower incisors too upright, enamel hypoplasia of tooth 21 (Figure 2); ectopic eruption of the left maxillary first permanent molar and resorption of the distal part of the second primary left molar (Figure 3). Cephalometric view showed retrognate mandible and maxilla (SNA=72.42, SNB=67.33) proclinated upper centrals I/ to /I=141.28) and Cl II skeletal problem (WITS=7.15) (Figures 4 and 5).
Figure 1. Extra-oral pictures at the age of 7 years and 2 months
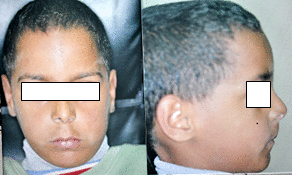
Figure 2. Intra-oral clinical views
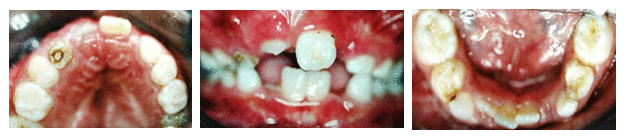
Figure 3. Panoramic X-rays at the age of 7 years and 2 months
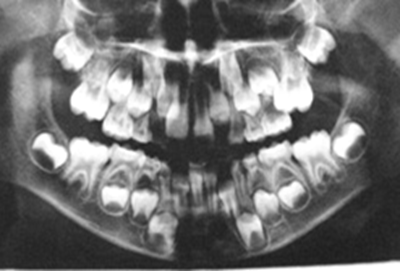
Figure 4. Cephalometric view at the age of 7 years and 2 months
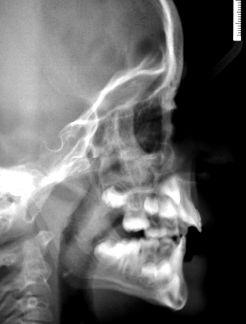
Figure 5. Cephalometric analysis at the age of 7 years and 2 months
Treatment The dental treatment included root canal treatment of tooth #73 due to an excessive caries lesion involving pulp tissue. (Figure 6) The treatment was performed in order to maintain arch length. Glass-ionomer restorations (Fuji IX by GC Japan) were performed on teeth #64, 73, 74, 83, tooth #52 was extracted; stainless steel crown was cemented on tooth #84 and fissure sealants were performed on teeth #85 and permanent first molars after full eruption. The early orthodontic treatment included space regainer after exfoliation of teeth #55, 65 (Figure 6).
Figure 6. Panoramic view during early orthodontic treatment at the age of 9 years old
The final orthodontic treatment performed at the age of 11 included serial extraction of primary teeth (canines and first molars) and of first premolars after eruption. A full orthodontic treatment was performed for two years (Figures 7 and 8). The profile at the age 13 years still showed a retrognathic mandible and maxilla (SNA= 72.9, SNB= 67.7, WITS=3.0) (Figures 9-11). The patient considered an orthognatic surgery procedure, but it was declined by the oral surgeons.
Figure 7. Orthodontic treatment
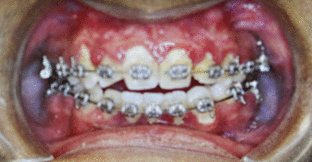
Figure 8. Panoramic view during orthodontic treatment at the age 13 years
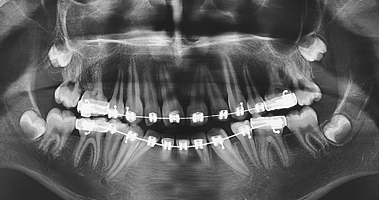
Figure 9. Extra-oral views at the age 13 years
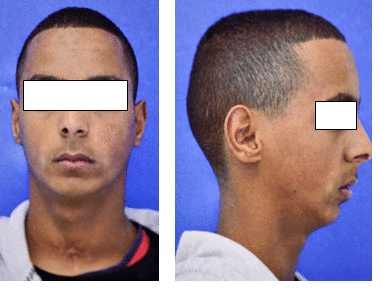
Figure 10. Cephalometric view at the end of orthodontic treatment
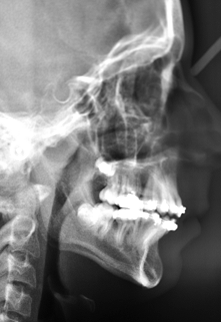
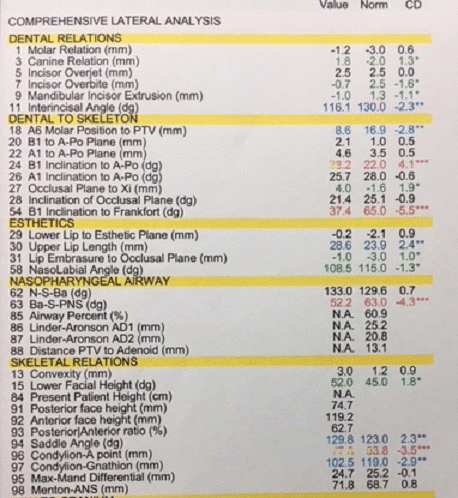
Figure 11. Cephalometric analysis at the age of 13 years
Discussion
Management of dental patients with special health needs In the guidelines of the AAPD for patients with special needs,11 dental care requires special knowledge, awareness, and special attention.
Although N.A. is in a favorable health condition, he is defined as suffering from a chronic condition that puts him in the category of children with special needs.
According to the guidelines, care of the group of SCHN (Special Care Health Needs) also includes children with isolated oro-facial complications such as Amelogenesis imperfecta, Dentinogenesis imperfecta and cleft lip and palate.11 These children are exposed to increased risk of oral diseases; therefore, it is crucial to establish a preventive dental home.11,12 Dental services are among the best health services required for children with special needs.12
The presented case describes a relatively restricted oro-facial anomaly, but it required involvement of multidisciplinary attention. N.A had coordinated visits and consultations at the cleft lip and palate department, pediatrics, ENT, speech therapy, orthodontics, plastic surgery and maxillofacial surgery. There were also psychological aspects in the context of aesthetics, appearance, and language development.
Another consideration in this case is the economic consideration. N.A. comes from a lower socioeconomic status and his parents found it extremely difficult to meet the expenses of the treatment. Nevertheless, by establishing trust and dedication, he has finished the necessary dental treatment and meticulous supervision and was ready for orthodontic treatment.
DDE - developmental defects of enamel DDE is defined as an expression of interference in the matrix positioning and mineralization of the dental tissues during development.
Defects may be local (single tooth or several teeth) or widespread (affecting dental groups that develop during the disturbance).
In NA case the etiology of enamel hypoplasia of upper central permanent incisor was difficult to determine. No reference was found to describe any relation between PRS and enamel hypoplasia. Soon after birth, N.A. suffered from breathing difficulties, nutrition disorders and recurrent fevers, which may have been the reason for the enamel defects. On the other hand, this reason seems less likely, because it would have been expecting to see similar defects on other developing teeth in the same period. Hence, the reason may be trauma to the primary incisors, aggressive intubation, or hidden cleft. N.A. underwent several surgical treatments under general anesthesia (cleft repair, surgical tubing ears etc.). Restoration of the lesions has created smooth and uniform surfaces, which provided ability to keep better hygiene and aesthetic appearance.
To control pain and anxiety with minimal suppression of consciousness, the option of using a combination of inhalation sedation (N2O/O2) with hydroxyzine (Otarex) was chosen. This accepted method enables the patient to keep an open airway and respond to verbal and physical stimulations.13 Pulse rates and oxygen saturation values were monitored by a pulse oximeter and were normal.13,14 During several appointments, the patient's initial suspicion and anxiety disappeared gradually.
Caries prevention N.A was considered at high risk for caries. Recommended preventive instructions included daily fluoride rinses, fluoride tooth paste, flossing, low carbohydrate diet and periodic professional prophylaxis and fluoride varnish application. This has been particularly accentuated during the orthodontic treatment.15
Glass Ionomer (GI) restorations GI is an appropriate restorative material for primary teeth. Over the years, these improved materials are more comfortable to use, with better erosion resistance and have greater strength.16 Their advantages are ability to chemically bond to tooth structures, low shrinkage, reasonable biocompatible with pulp tissue, anti-cariogenic property through fluoride release, and hydrophilic. The disadvantages are minor -reduced adequate strength and toughness, abrasion, high initial solubility, and aesthetics.16–18 We used a method of heat curing the GI during setting, thereby significantly increasing the surface hardness and the resistance to erosion.19–21
Ectopic eruption of maxillary first permanent molar (MFPM) Ectopic eruption of first permanent molar (FPM) is more common in the maxilla. It may absorb the distal roots of the second primary molars. According to a review by Kennedy and his colleagues, incidence of ectopic MFPM is 3-4% higher in siblings and children with cleft lip or palate (CLP).22 Bjerklin found that the incidence is 4 times more common in children with CLP, compared to children without CLP.23 Mooney and his colleagues reported that children with ectopic FPM had at least one additional dental anomaly, such as infra occlusion of primary molars and CLP.24 Indeed, combinations of these phenomena (ectopic eruption, cleft palate, enamel hypoplasia) were found in N.A. Larson et al. reported a 57% incidence of ectopic eruption in children with Pierre Robin Sequence and malformed teeth, similar to children with large clefts and without PRS.25 The study group included 109 children with cleft palate, but only 14 were diagnosed as PRS. Often, the eruption time of the MFPM is delayed. This phenomenon is either uni, or bi-lateral. The etiology is controversial. Spontaneous correction (jump) occurs in 66% but is much lower in CLP cases. In the case of N.A. tooth #26 is in the "hold" position. The decision of the age whether the ectopic tooth is reversible or irreversible is between 7 and 8 years.26 By the time the treatment has begun, tooth #65 exfoliated spontaneously and it was necessary to regain space. That is the reason why early orthodontic treatment started.
Orthodontic treatment – aim and appliances A high percentage of hypodontia was described for PRS children, 32.9–42% 27-28 mainly in the micrognathic and retrograde mandible. In our case no hypodontia was observed. The early loss of #65 in the severe crowding of the upper jaw resulted in loss of space for the second premolar. This indicated early interceptive orthodontic treatment to prevent rotation and cross bite of the FPM and palatal eruption of the premolar. Kennedy et al. suggested removable appliance combined with extra oral head gear, which is considered an efficient mean for distalization of FPMs.22 In N.A. case the treatment included a combination of a fixed upper plate and a cervical restraint because the use of a fixed appliance less depends on patient compliance. On the lower jaw a 2×4 appliance was used for proclination of the incisors. The final orthodontic treatment included serial extractions due to the discrepancy between arch length in both jaws and teeth size and full brackets for both jaws.
Summary
This case report describes dental treatment of a child with Pierre Robin Sequence, which is a chronic systemic condition, mainly affecting the head and neck. The child was defined as high caries risk case. Therefore, in addition to restorative treatment, under inhalation and pharmacological sedation, caries prevention program was adopted. Compliance of the child and his family improved significantly along the treatment and the follow-up period. Following the dental treatment, orthodontic treatment was adjusted to his abilities combined with meticulous recall appointments of 3-6 months for examination, prophylaxis and fluoride treatments. Although the orthodontic treatment showed good results, the effect of PRS on the retrograde mandible remained, but the esthetics were improved. This case report demonstrates the importance of early intervention in children with PRS and the need for a multidisciplinary team work in order to give these patients a better quality of life.
References
- Breugem CC, Evans KN, Poets CF, et al. Best practices for the diagnosis and evaluation of infants with Robin sequence- A clinical concensus report. JAMA Pediatr. 2016;170: 894–902.
- Bush PG, Williams AJ. Incidence of the Robin Anomalad (Pierre Robin syndrome). Brit J of Plast Surg. 1983;36: 434–437.
- Printzlau A, Andersen M. Pierre Robin sequence in Denmark: a retrospective population-based epidemiological study. Cleft Palate Craniofac J. 2004;41: 47–52.
- Williams AJ, Williams MA, Walker CA, Bush PG. The Robin anomalad (Pierre Robin syndrome) a follow up study. Arch Dis Child. 1981;56: 663–668.
- Evans KN, Sie KC, Hopper RA, et al. Robin Sequence: From diagnosis to development of an effective management plan. Pediatrics. 2011;127: 936–948.
- Gorlin RJ, Cohen MM, Hennekam RCA. Syndromes of the Head and Neck. Oxford Monographs on Medical Genetics No. 42. 4th ed. Oxford: Oxford University Press, 2001: 860–864.
- van der Haven I, Mulder JW, van der Wal KG, et al. The jaw index: new guide defining micrognathia in newborns. Cleft Palate Craniofac J. 1997;34: 240–241.
- Hong P, Kearns D. Airway characteristics of infants with Pierre Robin sequence who undergo mandibular distraction osteogenesis. Ear Nose Throat J. 2015;94: E25–E29.
- Godbout A, Leclerc JE, Arteau-Gautier I, Leclerc LD. Isolated versus Pierre Robin sequence cleft palate: are they different? Cleft Palate Craniofac J. 2014;51: 406–411.
- Suri S, Ross RB, Thompson BD. Craniofacial morphology and adolescent facial growth in Pierre Robin Sequence. Am J Orthod Dentofacial Orthop. 2010;137:763–774.
- AAPD Guideline on Management of Dental Patients with Special Health Care Needs. Reference Manual. 37;15/16:166–171.
- Crall JJ. Improving oral health for individuals with special health care needs. Pediatr Dent. 2007;29: 98–104.
- Malamed SF. Introduction to conscious sedation. In: SF Malamed, (ed). Sedation, a Guide to Patient Management. 4th ed. Missouri, MO: Mosby, 2003.
- Guidelines for treatment under sedation and general anesthesia in dentistry. Ministry of Health, Israel.
- Opsahl Vital S, Haignere-Rubinstein C, Lasfargues JJ, Chaussain C. Caries risk and orthodontic treatment. Int Orthod. 2010;8: 28–45.
- American Academy of Pediatric Dentistry. Guideline on pediatric restorative dentistry. Pediatr Dent. 2011–2012; 33: 205–211.
- Croll TP, Nicholson JW. Glass ionomer cements in pediatric dentistry: review of the literature. Pediatr Dent. 2002;24: 423–429.
- Berg JH. Glass Ionomer cements. Pediatr Dent. 2002; 24: 430–438.
- Ten Cate JM, Van Duinen RN. Hypermineralization of dentinal lesions adjacent to glass-ionomer cement restorations. J Dent Res. 1995;74: 1266–1271.
- Kleverlaan CJ, van Duinen RN, Feilzer AJ. Mechanical properties of glass ionomer cements affected by curing methods. Dent Mater. 2004;20: 45–50.
- van Duinen RN. New approach for handling glass ionomers in restorative dentistry. Refuat HapehVehashinayim. 2011;28: 8–13, 68.
- Kennedy D, Patrick K. The clinical management of ectopically erupting first permanent molars. Am J Orthod Dentofac Orthop. 1987;92: 336–345.
- Bjerklin K. Ectopic eruption of maxillary first permanent molar. An epidemiological, familial, aetiological and longitudinal study. Swed Dent J. 1994;18: 1–66.
- Mooney GC, Morgan AG, Rodd HD, North S. Ectopic eruption of first permanent molars: presenting features and associations. Eur Arch Paediatr Dent. 2007;8: 153–157.
- Larson M, Hellquist R, Jakobsson OP. Dental abnormalities and ectopic eruption in patients with isolated cleft palate. Scand J Plast Reconstr Surg Hand Surg. 1998;32: 203–212.
- Bjerklin K, Kurol J. Ectopic eruption of the maxillary first permanent molar: etiologic factors. Am J Orthod. 1983;84: 147–155.
- Antonarakis GS, Suri S. Prevalence and patterns of permanent tooth agenesis in patients with nonsyndromic Pierre Robin sequence. Am J Orthod Dentofacial Orthop. 2014;145: 452–460.
- Anderson EM, Feragen KB, Milaksen D, et al. Bilateral Hypodontia in adolescents with Pierre Robin sequence. Cleft Palate Craniofac J. 2015;52: 452–457.



