Home / Journal / Clinical & Medical Cases
Venous Thoracic Outlet Syndrome in Three Greek Children: a Single-Centre Experience
Thoracic Outlet Syndrome thrombosis adolescents thrombophilia Doppler scanning
Athina Dettoraki, Georgios Charalampopoulos, Aikaterini Michalopoulou, Nikolaos Liassis, Evangelia Lykopoulou, Dimitrios Maras, and Helen Pergantou
DOI: 10.31532/ClinMedCases.2.1.001 31 Jan 2021
Abstract
Thoracic outlet syndrome (TOS) is underdiagnosed in children/adolescents. We describe three cases of children/adolescents with TOS diagnosed within one year in our Haemostasis and Thrombosis Unit: 1) a 14-year-old girl with sudden onset of left arm oedema- thrombosis of the left subclavian vein and filling defect in both subclavian veins due to an elongated C7 transverse process, 2) a 13-year-old swimming champion with sudden onset of right arm oedema and 3) an eight-year-old girl with left arm discomfort (already on anticoagulation due to cerebral sinovenous thrombosis) and complete outflow interruption of the left subclavian vein. All three girls have been on anticoagulation for 18, 6 and 4 months respectively without symptoms. Conclusion: These three cases underline physicians TOS awareness concluding in diagnosing in children/ adolescents and demonstrate a clinically satisfying outcome of pediatric TOS with initially conservative treatment, surgery planning and continuing follow-up.
Keywords
Thoracic Outlet Syndrome, thrombosis, adolescents, thrombophilia, Doppler scanning
Introduction
Thoracic Outlet Syndrome (TOS), a clinical condition affecting shoulder and neck anatomical regions, constitutes of various diverse disorders that result in the compression of the neurovascular bundle exiting the thoracic outlet. The thoracic outlet is an anatomical area in the lower neck defined as a group of three spaces between the clavicle and the first rib through which several important neurovascular structures pass. These structures include the brachial plexus, subclavian artery, and subclavian vein.1 Three main forms in decreasing prevalence are neurogenic, venous and arterial TOS.2 Compression of the area causes a constellation of distinct symptoms, which may include fatigue, upper extremity pallor, cyanosis, paresthesia, numbness, limb coldness, heaviness, muscle weakness, motor deficits, muscle atrophy, and pain.1,3 It should be stressed that the predominant symptoms of venous TOS (vTOS) or Paget-Schroetter Syndrome are swelling and cyanosis of the arm. vTOS commonly presents with hypertrophied anterior scalene and subclavius muscles, as patients are typically younger and more muscular.2 Symptoms of paresthesia and pain suggest neurogenic TOS which can accompany vTOS.
In the general population, 4–10% of deep vein thrombotic events (DVT) involve upper extremities, including vTOS. Primary upper limb DVTs are idiopathic, contributing to 20% of total number of upper extremity DVT cases. Secondary upper limb DVTs occur mostly due to systemic diseases, venous catheter insertion procedures and vTOS.4 TOS can be related to either congenitally, traumatically or functionally acquired causes, like vigorous, repetitive sporting activity.5 Volleyball or swimming, involving frequent elevation of the arms, can be the precipitating cause of vTOS. The typical patient is young, athletic and might even develop symptoms after a rigorous work out leading to thrombosis as described by the term "effort thrombosis".2 Complications include symptomatic pulmonary embolism, post-thrombotic syndrome and thrombotic recurrence.6 TOS is a diagnosis that in several cases may be mistakenly considered as idiopathic upper extremity DVT, if not being investigated with methods sensitive and indicative of TOS.
Generally, this condition occurs in adult patients between the age of 20–50 years,7 with female to male ratio of 3:1.8 TOS also occurs in young children and teenagers but diagnosis is often missed because it is not commonly thought of as a disorder that affects children. The typical neurovascular compressive symptoms of numbness or paresthesia caused by upper extremity elevation may not be present in younger patients, who may simply describe symptoms of heaviness or dull sensation in the arm or shoulder region. In addition, children are likely to attribute their symptoms to simple muscle strain.8 Therefore, TOS remains underdiagnosed in the paediatric population.
History and clinical examination are important during clinical evaluation. Physical examination should include measuring the circumference of the involved arm and forearm and comparing these measurements to those of the uninvolved side. Clinical suspicion can then be confirmed with provocative physical examination maneuvers, radiography, and/or vascular studies. Duplex ultrasound (US) examination is indicated as a first-line study [9]. Dynamic assessment of the vessel compression with abduction of the arm can be performed with US. However, because of the operator dependency and the complex anatomy of this region, US is not the definite modality for evaluating thoracic outlet syndrome. MRI and MR angiography are useful in this process.10
Given the wide range of multi-factorial etiopathologies, it makes sense that best-practice treatments for TOS follow a comprehensive and multi-disciplinary approach. Management options can include lifestyle modifications, pain management, anticoagulation treatment, physical therapy, rehabilitation and finally surgical correction. It should be noted that while physical therapy is a modality for treating neurogenic TOS, it is of no help for venous or arterial TOS. Altogether, treatment aims to prevent symptom progression and thrombosis recurrence. Chronic venous insufficiency or persistent symptoms may require subsequent surgical decompression.5
Case Report
Here we report three female patients with vTOS diagnosed within one year in our Thrombosis and Haemostasis Unit and managed initially in a conservative manner with the aim of preventing symptoms progression.
Case #1
Firstly, we describe the case of a 14-year-old girl who presented to the paediatric department of a regional hospital in a Greek island with sudden onset of oedema of her left arm. Not trauma or other precipitating event, family history of thrombophilia or prior medical history of pain/oedema in the relevant arm was previously reported since the patient remained a healthy adolescent till the event. She was attending physically vigorous training courses (volleyball) for last five months prior to onset of symptoms. Ultrasound imaging revealed thrombosis of the left axillo-subclavian vein. Chest CT scanning did not show any malformation with potency of causing venous blockage, apart from elongated C7 transverse process. Low molecular weight heparin (LMWH) was administered to the patient as anticoagulation therapy. Systemic and inflammatory diseases were excluded as probable diagnoses through relevant laboratory investigation. The patient was referred to our Unit, five days after initial symptoms. Swelling was ameliorated, however the girl was still complaining of pain. Patient’s anticoagulation therapy was switched to warfarin per os. Thrombophilia testing, undertaken after the initiation of anti-coagulation, revealed heterozygosity for FVLeiden, homozygosity for MTHFR-C677T polymorphism with normal values of homocysteine and low protein S (PS) values (PS=55%, normal values 60–140%), which will be evaluated again after the cessation of anticoagulation therapy. Venous duplex scanning (VDS) was performed by an experienced radiologist that dynamically investigated the arms in abduction and external rotation positions (Elevated Arm Stress Test-EAST) (Fig. 1). Thrombosis of the left axillo-subclavian vein was assessed and a filling defect in both subclavian veins was demonstrated due to an elongated C7 transverse process compressing the brachial plexus thus, establishing the diagnosis of TOS.
Figure 1. Upper extremity venous duplex scanning depictive of complete thrombosis of the left subclavian vein (arrow) with absence of blood flow on colour Doppler.
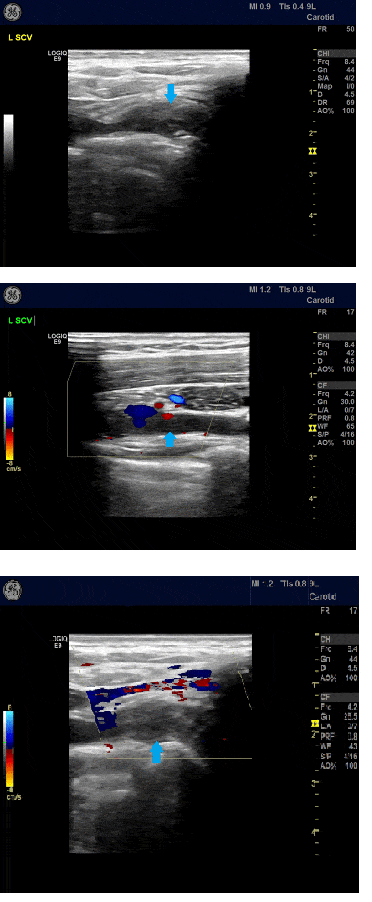
MRI and MR angiography (MRA) of the upper arm were confirmative of the diagnosis. Initially, conservative treatment was applied, i.e. instructions to rest and avoid heavy physical activities, in addition to antithrombotic treatment with warfarin. A second ultrasound imaging test at six months after diagnosis showed improvement of recanalization at the site of the initial thrombus with a partial remnant occlusion of the left axillo-subclavian vein (Fig. 2). Eighteen months after the occurrence of the thrombotic episode, the patient is still on anticoagulants. Available treatment options (anticoagulation therapy, lifestyle modifications, surgery) were discussed with the patient and her parents. A surgical procedure of first rib resection and anterior scalenectomy is planned for this adolescent as soon as possible. Diagnostic investigation and identification of the anatomical cause of TOS have been completed, and it is assured that the quality of life of the patient will be improved by surgical treatment. However, because of her age (she’s about to be sixteen years old) she will be followed up from now on in an adult hospital and due to COVID-19 pandemic such surgeries have been postponed.
Figure 2. Upper extremity venous duplex scanning depictive of partial thrombosis of the left axillary vein (arrow) causing a filling defect in the venous lumen on colour Doppler. Spectral Doppler waveforms show absence of the normal respiratory phasicity of the venous flow in the left axillary vein due to proximal subclavian vein thrombosis (image on the right) in contrast to normal phasicity of the blood flow in the right axillary vein.
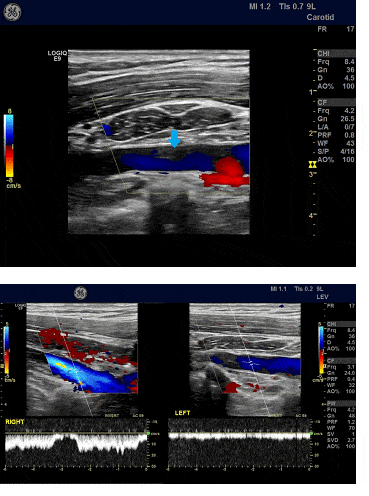
Case #2
Eight months later, a 13-year-old right-handed girl was referred to the pediatric department of our hospital with sudden onset of oedema and pain of her right arm. The patient was an otherwise healthy adolescent, as she had been a swimming champion. Due to increased awareness, a VDS was performed directly and thrombosis of the right subclavian vein was assessed. EAST was not performed during the acute phase of thrombosis. Diagnosis of TOS was posed later through the appropriate dynamical investigations that revealed a filling defect in both subclavian veins. MRI and MRA of the upper arm confirmed the diagnosis. Thrombophilia testing (off anticoagulation) revealed borderline low protein S values (PS=62%) and heterozygosity for MTHFR-C677T polymorphism with normal homocysteine values. Anticoagulation initially with LMWH subcutaneously and then with warfarin orally was administered. The girl has been on anticoagulation for six months with elimination of symptoms (e.g. pain and oedema). Surgical procedure is also planned for this patient.
Case #3
Finally, two months later there was a third case of an eight-year-old girl who had already been on anticoagulation for eight months after cerebral sinovenous thrombosis following herpetic gingivostomatitis. Because of gradual onset of oedema and pain of her left arm and increased awareness after the aforementioned cases, a VDS with dynamic investigations was performed immediately, which revealed complete outflow interruption of the left subclavian vein and milder outflow interruption of the right subclavian vein during EAST. Thrombophilia screening had been undertaken in the past before the initiation of anticoagulants and had revealed homozygosity for MTHFR-C677T polymorphism with normal homocysteine values. She has been on anticoagulation for one year (four months since TOS justification) with no symptoms.
Discussion
The clustering of TOS cases in a short period of time in our Unit was probably due to increased awareness of paediatricians and clinical suspicion of TOS in young healthy adolescents with symptoms from the upper extremities. Prompt TOS recognition and treatment application provide for the greatest probability of optimal recovery. Specifically, diagnosis of TOS should be considered when a child or adolescent presents with neck and shoulder discomfort, hand numbness and upper limb weakness. However, it is particularly important for parents and clinicians not to arbitrarily conclude that this is a condition of simple muscle strain [8]. Unfortunately, non-specific symptoms and challenging diagnosis may delay treatment application and increase the risk of complications. Despite the advances made, substantial controversy remains regarding the diagnosis. Challenges associated with definite diagnosis complicate decision-making on beneficial treatment application.
Availability of therapeutics is also another challenge in TOS treatment. Most vascular surgeons have adopted an aggressive approach, 11 since the most common reason for acute DVT in such patients is the underlying compression of the axillary-subclavian vein by the first rib. So, an endovascular and/or surgical approach in order to potentially relieve the compression and provide excellent long-term results have been adopted by most surgeons.12 Recently, a few case series have documented surgical treatment of TOS in children with unusual anatomy, including abnormal first ribs, cervical ribs, fractured ribs and abnormal tendon insertions.12–14. Surgical decompression provides durable treatment success in children with most subtypes of thoracic outlet syndrome.12
Concerning case #1, as the anatomical cause of TOS (an elongated C7 transverse process compressing the brachial plexus) has been identified, a surgical procedure is planned as soon as possible. It has already been mentioned that our patient needs a first rib resection and anterior scalenectomy- the subclavian tendon, which lies right next to the subclavian vein, should be cut. Compression of the subclavian vein is also present in the right arm, so prophylactic surgery on the right side should be considered, as well. In this case, the adolescent will be anticoagulated until the proposed surgery is performed, probably bilaterally. Until then, the patient is recommended not to play volleyball or do exercises involving elevation of her arms.
In case #2, competitive swimming seems to be the cause of vTOS, as it involves repetitive elevation of the arms (like volleyball). Our patient is recommended to refrain from competitive swimming until she is operated upon. Both arms had been evaluated for venous compression and TOS was found bilaterally. This adolescent probably needs to have a first rib resection as well.
Both cases #1 and #2 illustrate classic causes for effort thrombosis- volleyball and swimming. Without rib resection, recurrent thrombosis rates range from 25% to 75%. Most patients with effort thrombosis do not have a bone abnormality- it is usually the subclavian tendon, anterior scalene or the first rib which compresses the vein, a fact usually associated with activity.2 Case #1 also revealed positive thrombophilia testing (heterozygosity for FVLeiden, homozygosity for MTHFR-C677T polymorphism and low protein S values), which consists of a precipitating factor for thrombosis. Case #2 revealed borderline low protein S values as well, which will be evaluated again after the cessation of oral anticoagulation therapy.
On the contrary, case #3, the eight-year-old with complete obliteration of the subclavian vein with elevation, cannot be considered as representative of effort thrombosis. This patient is also advised to avoid activities involving repetitive elevation of her arms so as to prevent thrombosis of the subclavian vein. Both arms have been evaluated for venous compression, as this entity is frequently bilateral and milder obliteration of right subclavian vein was also found. This patient probably has a hypercoagulable state (homozygosity for MTHFR-C677T polymorphism possibly combined with some other factor) and TOS is not effort-associated, so she could not be a candidate for rib resection. Management could comprise either long term anticoagulation or surgical thoracic outlet decompression. However, as this girl grows older, her compression may be relieved, so she might need only anti- coagulation. Some children, like in this case, have no definite anatomical cause for vTOS. Therefore, early surgical therapy may not be necessary. Skeletal development will be gradually completed as the patient grows up and the compression will probably be ameliorated. In these cases, conservative handling (“wait and see”) plus anticoagulation is also an acceptable alternative treatment.
It has already been mentioned that physical therapy is not an option for vTOS. The patients should avoid activities that involve repetitive elevation of the arms, such as swimming, volleyball, and baseball pitching as well as using the arms overhead. It should be emphasized that two out of our three patients were involved in physical activities (competitive swimming and volleyball) that could be the etiology of their symptoms.
The patients presented in this article are initially managed in a less
aggressive manner so that the symptoms could recede. Further studies
evaluating the long-term outcomes of conservative treatment in children
with TOS and DVT are required. The optimal duration of anticoagulation
therapy in these patients is still to be defined. Our intention regarding
the three girls with TOS and DVT is to continue anticoagulation until the
anatomical complication resolves, either surgically or in the context of
skeletal maturation, conservatively. All three patients are still on
treatment with warfarin per os, in regular follow-up visits including
clinical examination and VDS, almost always accompanied with clinical
consultation by the vascular surgeon. The conservative management of these
three girls with TOS was proved successful and well tolerated. The first
two cases are planned for surgery, while the third one is given the time
for the skeletal development to be completed, waiting for the vascular
surgeon to determine the appropriate type and timing of surgical
intervention, if necessary.
Conclusion
Identification of TOS is complex. However, medical practitioners, mainly paediatricians, should include TOS in the differential diagnosis in cases of shoulder and upper extremity pain manifestation so that patients are timely directed to prompt therapeutic intervention.
Immediate TOS diagnosis and initiation of treatment provide the greatest probability of excellent recovery. These three cases, presented in this paper, demonstrate a favorite clinical outcome of paediatric TOS with uncommon underlying etiology, initially managed conservatively. Elimination of symptoms and improvement of quality of life is the primary goal regarding the treatment of TOS in children, not forgetting the possibility of future surgical correction in the proper time for each patient.
Acknowledgements
We thank the families involved in this study and particularly, the children that helped us with their cooperation.
Informed consent
Informed consent was obtained from all individual participants included in the study.
References
- Jones MR, Prabhakar A, Viswanath O, et al. Thoracic Outlet Syndrome: A Comprehensive Review of Pathophysiology, Diagnosis, and Treatment. Pain Ther. 2019; 8(1): 5–18.
- Archie AM, Rigberg D. Vascular TOS—Creating a Protocol and Sticking to It. Diagnostics (Basel). 2017; 7(2): 34.
- Mustafa J, Asher I, Sthoeger Z, et al. Upper Extremity Deep Vein Thrombosis: Symptoms, Diagnosis, and Treatment. Isr Med Assoc J. 2018; 20(1): 53–57.
- Menon D, Onida S and ADavies AH. Overview of venous pathology related to repetitive vascular trauma in athletes, J Vasc Surg Venous Lymphat Disord 2019; 7(5): 756–762 doi: 10.1016/j.jvsv.2019.03.012. Epub 2019 Jun 21.
- Chang K, Graf E, Davis K, et al. Spectrum of Thoracic Outlet Syndrome Presentation in Adolescents. Arch Surg. 2011;146(12): 1383–1387.
- Heil J. Miesbach W. Vogl T, et al. Deep vein thrombosis of the upper extremity. Dtsch Arztebl Int. 2017; 114: 244–249.
- Hussain MA, Al—Omran M. Vascular Thoracic Outlet Syndrome. Semin . Thorac Cardiovasc Surg Spring. 2016, 28 (1): 151–157. doi: 10.1053/j.semtcvs.2015.10.008. Epub 2015 Oct 28.
- Rehemutula A, Zhang , Chen L, et al. Managing pediatric thoracic outlet syndrome. Italian J Pediatr. 2015; 41: 22
- Martins Zucker E, Ganguli S, Ghoshhajra B, et al. Imaging of venous compression syndromes. Cardiovasc Diagn Ther. 2016; 6(6): 519–532.
- Chavhan G, Batmanabane V, Muthusami P, et al. MRI of thoracic outlet syndrome in children. Pediatr Radiol. (2017); 47: 1222–1234,
- Spivack A, Troutman D, Dougherty M, et al. Changing Strategies to Treat Venous Thrombotic Occlusions of the Upper and Lower Extremities Secondary to Compressive Phenomena. Vasc and Endovascular Surg. 2013; 47(4): 274–277.
- Bendgude Matos JM, Gonzalez L, Kfoury E, et al Outcomes following operative management of thoracic outlet syndrome in the paediatric patients. Vasc. 2018; 0(0): 1–8.
- Rochlin D, Orlando M, Likes K, et al. Bilateral first rib resection and scalenectomy is effective for treatment of thoracic outlet syndrome J Vasc Surg. 2014; 60: 185–190.
- O'Brien PJ, Ramasunder S, & Cox MW. Venous thoracic outlet syndrome secondary to first rib osteochondroma in a pediatric patient. J Vasc Surg. 2011; 53(3): 811–813.



